Few transitions in medicine carry as much weight as the one from medical student to first-year resident. One day you are standing at the edge of a code, watching an attending run the resuscitation while you quietly observe. The next, you are the one in charge — pager going off, nurses looking to you, and a patient in cardiac arrest. That shift happens faster than most trainees expect, and the gap between knowing ACLS algorithms on paper and executing them under real pressure can feel enormous.
The good news is that this gap is closeable, and the tools to close it are more accessible than ever. Building genuine ACLS confidence during your first clinical year is not about memorizing every algorithm perfectly — it is about developing the leadership mindset, communication habits, and procedural fluency that allow you to function at your best when the stakes are highest. This guide is written for those at exactly that inflection point: finishing medical school, entering residency, or stepping into a clinical role where code team leadership is now part of the job.

Research confirms what most interns already suspect: the transition is harder than expected. Studies show that nearly 98.6% of residents report feeling uncertain or lacking confidence when asked to lead a multidisciplinary code team. In a separate survey, only 52.1% of first-year residents felt genuinely prepared to lead a cardiac arrest team, while more than half worried they had made errors during actual resuscitation events.
These numbers are not meant to alarm — they are meant to normalize. Feeling underprepared does not mean you are inadequate. It means you are like virtually every other trainee who has come before you. What separates those who grow quickly from those who stay stuck in anxiety is a proactive approach to both clinical knowledge and team leadership skills. According to research published in the Journal of Brown Hospital Medicine, residents who received structured leadership training showed significant improvements in team dynamics and code performance compared to those who relied on experience alone.
Understanding what you are walking into is the first step toward building real confidence. Most teaching hospitals designate the senior resident or on-call intern as the code team leader for in-hospital cardiac arrests. Depending on your specialty and institution, that role could fall to you within the first weeks of intern year. Knowing that — and preparing for it deliberately — changes everything.
ACLS certification gives you the algorithmic foundation every code requires. You learn to recognize shockable versus non-shockable rhythms, manage airway and ventilation, sequence medications appropriately, and identify reversible causes through the H's and T's. That knowledge is non-negotiable. But the certification itself is where preparation begins — not where it ends.
For students and early residents who are planning ahead, the timing and format of your ACLS certification matters. The medical student's guide to ACLS certification outlines why getting certified before you enter residency — rather than scrambling during orientation week — gives you a meaningful edge. You arrive with currency in the algorithms already, which frees up your mental bandwidth to focus on the leadership layer that residency actually demands.
Platforms like Affordable ACLS, founded by board-certified Emergency Medicine physicians, allow you to complete your certification entirely online, at your own pace, with unlimited retakes and immediate digital certification. At $99 for ACLS — with bundle discounts available — there is no reason to delay getting this credential in hand before your clinical responsibilities begin. The self-paced format means you can review the content as many times as needed to genuinely internalize it, not just pass a test.
There is a meaningful difference between recognizing an algorithm when you see it and being able to execute it flawlessly while someone is performing chest compressions, a nurse is asking about medication dosing, and a respiratory therapist is positioning for intubation. The goal for your first clinical year is to internalize the core ACLS algorithms to the point of automaticity — where the framework runs in the background while your conscious attention manages the team dynamics in the foreground.
The primary algorithms to own completely are ventricular fibrillation and pulseless ventricular tachycardia (VF/pVT), pulseless electrical activity (PEA), asystole, bradycardia with a pulse, and tachycardia with a pulse. For each one, you should be able to articulate the immediate steps, the medication sequence, the defibrillation strategy if applicable, and the most common reversible causes to consider. Review the key changes in ACLS guidelines for 2025 to ensure your knowledge reflects the most current evidence — guidelines evolve, and outdated information can affect clinical decision-making in ways that matter.
One practical approach used by strong trainees: after each simulation or real code exposure, mentally walk back through the sequence. What happened first? What was called correctly? Where did the team lose the thread? This kind of structured reflection accelerates retention far more than passive review. For more structured study strategies, the 10 essential study tips for ACLS certification offer a practical framework that applies both to exam preparation and ongoing clinical reinforcement.
Running a code is not primarily a cognitive exercise — it is a leadership exercise. The physician leading the resuscitation is not the one performing compressions, pushing medications, or bagging the patient. The leader's job is to direct, delegate, synthesize information, make decisions, and keep the team operating as a coherent unit. That is a fundamentally different skill set than knowing the algorithms, and it requires its own kind of development.
Effective code team leaders share several consistent behaviors. They position themselves at the foot of the bed to maintain visual oversight without being physically in the way. They speak clearly and calmly even when the situation is urgent. They explicitly assign roles rather than assuming someone will step up. And they use closed-loop communication — giving a direct order, hearing it repeated back, and confirming completion — to eliminate the ambiguity that causes errors. According to research published in BMC Medical Education, nearly half of resuscitation errors stem from poor teamwork and leadership rather than from gaps in clinical knowledge.
For a deeper dive into the specific language and scripts that make team communication effective during a code, the resource on ACLS team dynamics and communication scripts provides practical language you can adapt to your own style. The point is not to sound scripted — it is to have clear, reliable language patterns ready so that under stress, you default to structure rather than improvisation.
When you arrive at a code, the first minute is the most disorienting and the most consequential. Experienced leaders have a framework they apply immediately, which prevents the paralysis that comes from facing too many simultaneous inputs at once. Having your own version of this framework — practiced enough to be reflexive — is one of the most valuable things you can develop in your first clinical year.
A framework used by many strong code leaders: In the first 10 seconds, identify who is currently running the code and take command clearly. In the first 60 seconds, confirm that the fundamentals are in place — airway, compressions with full recoil at the right rate and depth, IV or IO access, and the monitor showing a readable rhythm. In the second 60 seconds, explicitly assign roles if they have not been established, confirm the crash cart is accessible, and ensure someone is capturing the timeline. By the two-minute mark, you should be managing the rhythm rather than reacting to it.
One underused tactic: designate a specific team member as your information liaison — someone who reviews the patient's chart, recent labs, and clinical context so you can ask direct questions rather than sorting through information yourself in real time. This keeps your attention where it belongs: on the resuscitation sequence and team performance. The mental preparation guide for your first real code covers this and other cognitive strategies that complement your algorithmic training.
Simulation is the single most effective tool for converting theoretical ACLS knowledge into functional clinical leadership. High-fidelity simulation creates the physiological stress response — elevated heart rate, narrowed attention, decision pressure — without actual patient consequences. Trainees who engage seriously with simulation during their early clinical year consistently outperform peers who rely on real code exposure alone.
According to research published on simulation-enhanced spaced learning for ACLS training, an interprofessional curriculum using spaced repetition improved both algorithm adherence and trainee confidence significantly. The key word is spaced — simulation done once at orientation is far less effective than simulation revisited at intervals throughout the year as your responsibilities evolve.
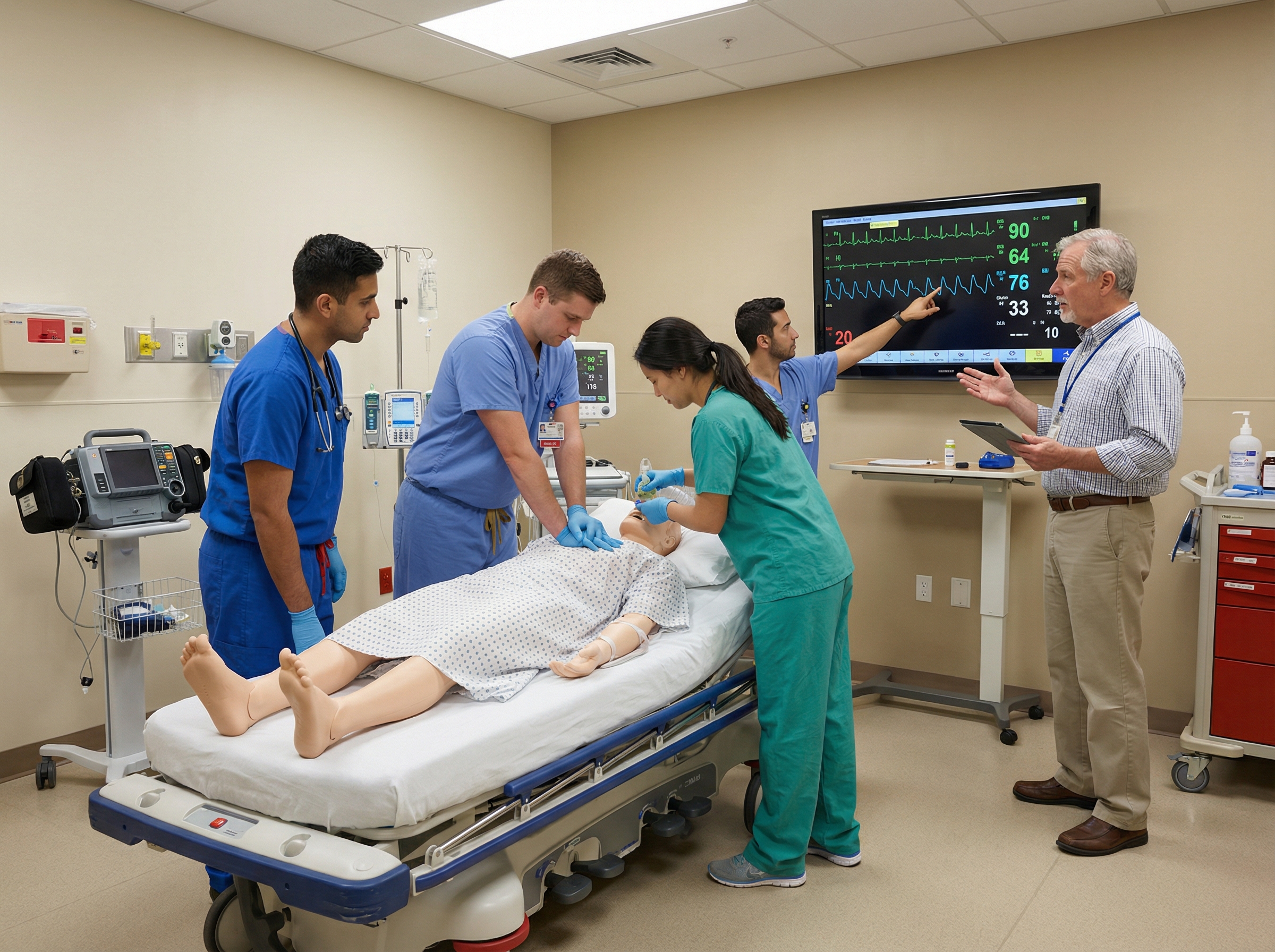
Most residency programs offer some form of mock code or simulation lab access. Use it deliberately. Ask your simulation faculty to put you in the team leader role specifically, even when it feels uncomfortable. Request debriefs focused on your communication and decision-making rather than just the clinical sequence. For more on how simulation translates to real-world performance, the resource on how simulation training enhances real-world resuscitation skills provides a strong conceptual framework for getting the most out of these experiences.
Clinical competence and psychological readiness are not the same thing, and neglecting the latter is one of the most common reasons otherwise knowledgeable trainees perform below their ability during high-stakes situations. The stress response during a code — elevated cortisol, tunneled attention, working memory compression — is physiological and affects everyone. The question is not whether it will happen to you, but what cognitive tools you have ready when it does.
One of the most effective strategies is pre-exposure mental rehearsal. Before going on call, walk through a code mentally in enough detail that you have already experienced it at some level. Who will you designate for compressions? What will you say to take command? What is the first rhythm you want to confirm? Athletes call this visualization. Surgeons call it pre-operative mental walkthrough. In emergency medicine, it is simply smart preparation. The result is that when the real event happens, your nervous system has a reference experience to draw on rather than encountering pure novelty.
Building confidence also means giving yourself permission to not know everything. Strong code leaders ask questions. They say "What rhythm are we seeing?" and "Does anyone have information about this patient's baseline?" out loud, because gathering information from the room is a leadership skill, not a sign of weakness. For more strategies on building clinical confidence as a new team member, the comprehensive resource on building confidence as a new code team member addresses both the practical and psychological dimensions of this transition.
Every code you participate in — whether as a team member or leader, whether it results in ROSC or not — is an educational event if you approach it that way. The trainees who develop fastest in their first clinical year are those who debrief deliberately and consistently, not just after bad outcomes but after every resuscitation event.
A structured post-code reflection does not need to be long. Three questions cover most of the important ground: What went well and why? What would I do differently? What do I need to review or practice before the next code? Answering those questions honestly and specifically — not vaguely — generates the kind of targeted improvement that compounds quickly over a year of clinical exposure.
Seek feedback from the nurses and respiratory therapists who were in the room. They have a view of the resuscitation that you do not — they can tell you whether your communication was clear, whether the team felt directed, and where the confusion or hesitation was visible. Their feedback is often more actionable than what you will receive from physician colleagues. According to expert guidance for residents leading codes, actively seeking interprofessional feedback after each event is among the highest-yield habits for accelerating code leadership development.
Residency is not a schedule that accommodates much flexibility. The demands of clinical rotations, overnight call, and didactic responsibilities leave limited time for certification preparation, which is exactly why the format and timing of your ACLS certification matters so much. Attempting to prepare for an in-person ACLS course during your busiest rotation is a setup for a stressful experience and suboptimal learning.
Online ACLS certification through Affordable ACLS allows you to work through the material in segments that fit your actual schedule — not an arbitrary fixed-date class. You can review a module during a quiet night shift, revisit the rhythm interpretation section before a cardiology rotation, or complete the final assessment when you genuinely feel ready rather than on a predetermined date. The immediate digital certification means your credential is in hand the moment you need it, without waiting for a mailed card. For residents specifically managing this balance, the comprehensive guide to balancing residency and ACLS certification provides practical strategies for making it work within the constraints of a demanding training program.
Unlimited retakes remove the high-stakes pressure of a single-attempt exam, which is particularly valuable when you are navigating a high-cognitive-load period of training. The goal is genuine mastery — not just passing — and the format supports that distinction. AHA and ILCOR compliance ensures the certification meets the standards required by hospitals, credentialing committees, and licensing boards.
The confidence you build during your first clinical year does not only serve you in that year. It establishes a pattern of clinical leadership that carries forward through every subsequent phase of training and practice. Residents who develop genuine code team leadership competency in intern year become the attendings who run resuscitations with calm authority. They become the educators who train the next generation of interns. They become the physicians who are called when a situation is complex and experience matters most.
Your ACLS certification is one piece of that foundation, but the mindset it represents — proactive preparation, commitment to team leadership, structured reflection after high-stakes events — is the part that scales. According to career guidance from clinical education experts, physicians who invest in genuine ACLS mastery early in training demonstrate measurably better team performance outcomes and professional confidence across their careers.
For those thinking beyond first-year certification toward a broader career development path, understanding how certifications stack and build on each other is worth planning deliberately. The resource on mapping your career path from BLS to ACLS and PALS provides a strategic framework for sequencing your credentials in ways that align with your specialty and practice setting goals.
If you are preparing for your first clinical year and want to arrive with genuine ACLS confidence, here is a concrete sequence that works:
The transition from student to code team leader is one of the most significant professional shifts you will make. The fact that you are approaching it proactively — rather than waiting to be thrown into it — means you are already doing the right things. The gap between where you are and where you need to be is real, but it is closeable, and every tool described in this guide is designed to help you close it faster.
ACLS certification gives you the algorithmic foundation. Leadership development gives you the team performance skills. Structured reflection gives you the compounding improvement that turns a challenging first year into a genuinely formative one. Your patients, your team, and your future self all benefit from that investment.
Affordable ACLS offers 100% online, self-paced ACLS certification starting at $99 — developed by board-certified Emergency Medicine physicians who understand exactly what clinical practice demands. With unlimited retakes, immediate certification, and AHA/ILCOR-compliant content, it is built for healthcare professionals who want genuine mastery on a schedule that respects the realities of training. Visit affordableacls.com or call 866-655-2157 to get started today.
.jpg)

