Few moments in clinical practice carry as much weight as a resuscitation event. The room is loud, the pace is unrelenting, and every second matters. Now add a family member standing at the foot of the bed — watching, grieving, hoping — and you have one of the most ethically and emotionally complex situations a healthcare provider will ever face.
Family presence during resuscitation (FPDR), also known as family-witnessed resuscitation, has been debated in emergency medicine and critical care for decades. What was once considered a disruption to clinical workflow is now increasingly recognized as a patient- and family-centered practice supported by a growing body of evidence. The 2025 American Heart Association guidelines continue to emphasize family-centered care as a core principle of resuscitation practice.
For ACLS-certified providers — whether you are an RN, PA, physician, paramedic, or respiratory therapist — understanding how to navigate FPDR is not just about clinical skill. It is about leading a high-performing code team with compassion, clarity, and professionalism. This article breaks down what the evidence says, how to structure your team's approach, and how to train effectively for these moments.
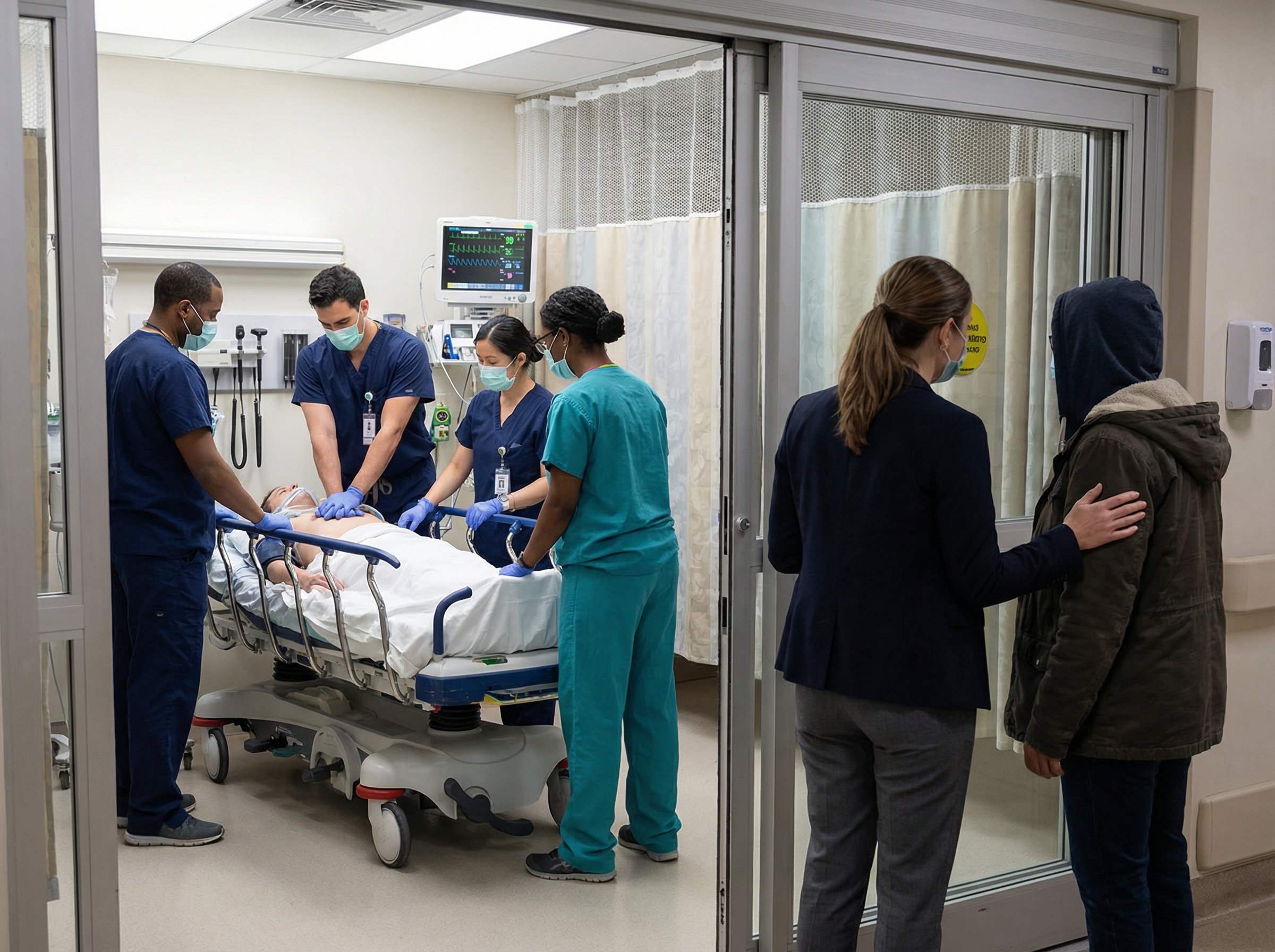
Family presence during resuscitation refers to the deliberate option offered to a patient's loved ones to witness resuscitative efforts — CPR, defibrillation, medication administration, airway management — as they are happening. This is distinct from accidentally walking in on a resuscitation. True FPDR is a structured, supported experience facilitated by a designated team member.
The concept gained traction in the 1980s when the Foote Hospital in Michigan began formalizing the practice after family members expressed a strong desire to be present. Since then, professional organizations including the American Association of Critical-Care Nurses (AACN) and the Emergency Nurses Association have formally endorsed family-witnessed resuscitation as an evidence-based practice when properly implemented.
Despite professional endorsement, implementation remains inconsistent across hospitals and healthcare systems. International research consistently shows that FPDR is practiced far less than guidelines recommend, largely due to provider concerns about team performance, family trauma, and lack of institutional policy. Understanding both the evidence and the barriers is the first step toward confident practice.
The research on FPDR has matured significantly over the past two decades, and the findings challenge many of the assumptions that keep it from being widely adopted.
One of the most compelling findings comes from a landmark study published in the New England Journal of Medicine examining family members of patients who experienced out-of-hospital cardiac arrest. Researchers found that family members who witnessed resuscitation had significantly lower rates of PTSD-related symptoms compared to those who did not witness CPR. The protective psychological benefit persisted at the one-year follow-up mark. Families who were present reported reduced anxiety, depression, and grief — and reported feeling they had done everything they could for their loved one.
This matters enormously for nurses, physicians, and other clinicians who work with grieving families long after the acute event. When families are excluded from the resuscitation room, unanswered questions and unresolved grief can linger for years. Witnessing resuscitation — even unsuccessful resuscitation — gives families a sense of closure and reinforces the reality of what occurred in a way that a bedside conversation afterward often cannot replicate. Understanding how nurses can help the grieving patient starts with recognizing that FPDR itself is one of the most meaningful forms of support a care team can offer.
The concern most often voiced by resuscitation providers is that family presence will distract the team, slow response times, or compromise the quality of CPR. A prospective randomized simulator-based trial published in PMC examined exactly this question. The findings were clear: while family presence was associated with modestly increased levels of perceived mental and temporal demand, it had no measurable negative effect on the quality of CPR. Chest compression rates, defibrillation timing, drug selection, and resuscitation duration were all unaffected by family presence.
A separate retrospective observational cohort study on in-hospital family-witnessed resuscitation reached similar conclusions — that key resuscitation processes and outcomes were not negatively affected when family members were present. The fear that FPDR derails clinical teams appears to be largely an assumption unsupported by the current evidence base.
That said, team performance under FPDR is not automatic. It depends heavily on preparation, role clarity, and having the right supporting structure in place — which is where ACLS training and team dynamics education become critical.
If the evidence supports FPDR and professional organizations endorse it, why is it still practiced so inconsistently? The barriers are real, and dismissing them without acknowledgment does a disservice to the clinicians raising them.
The single most important structural element of a successful FPDR program is the family facilitator. This person's role is to remain exclusively with the family throughout the resuscitation event. They are not involved in clinical care. Their entire focus is on the family members in the room.
According to implementation guidance from the Palliative Care Network of Wisconsin, the facilitator's responsibilities include offering comfort and emotional support, explaining interventions and medical terminology in plain language, monitoring the family's coping and readiness to remain in the room, and being prepared to escort family members out if their presence becomes disruptive to care.
The facilitator does not have to be a physician. In fact, chaplains, social workers, and experienced nurses are often ideally suited for this role. What matters is consistent training, not professional designation. The key criterion is that the facilitator must not step away from the family to assist with clinical tasks — their singular focus must remain on the family throughout the event.
Before bringing a family member to the bedside, the facilitator should conduct a brief assessment of the family's readiness. This includes evaluating emotional stability, cognitive ability to process what they are seeing, and the absence of behavioral contraindications such as substance intoxication or severe agitation. Most hospitals limit family presence to one or two members to maintain manageability for the facilitator and minimize disruption to the team.
Effective resuscitation requires clear role assignments, closed-loop communication, and a team leader who maintains situational awareness. These are the same competencies that enable a team to function well with family present. When ACLS team dynamics are strong, family presence adds complexity — but not chaos.
The team leader plays a particularly important role during FPDR. While managing the resuscitation algorithm, the team leader must also be aware of family presence and communicate with the facilitator as needed. Brief, professional narration of key interventions — delivered calmly and without editorializing — can help families understand what is happening without requiring the team to pause clinical activity. Using ACLS team communication scripts reinforces professionalism and keeps the family oriented while preserving team focus.
The most effective way to prepare for FPDR is through simulation training that incorporates a family presence scenario. Simulation training enhances real-world resuscitation skills precisely because it allows teams to rehearse high-stakes scenarios without actual patient risk. Running a mock code with a team member acting as a distressed family member in the room is one of the most effective ways to build comfort and identify gaps in team protocol before the real situation arises.
Sustainable FPDR programs do not happen through individual provider initiative alone. They require institutional commitment and a structured rollout. Here is a framework drawn from evidence-based implementation guidance.
Bring together representatives from nursing, medicine, social work, pastoral care, respiratory therapy, and ideally patient and family advisors. This group should develop the written FPDR policy and procedure, define facilitator training requirements, and build the program rollout plan. Including a diverse stakeholder group increases buy-in and ensures the policy reflects real workflow constraints.
A written FPDR protocol removes ambiguity from the decision-making process during an already stressful event. The protocol should specify which patients and settings are covered, how the facilitator is identified and activated, the family assessment criteria used, how many family members may be present, and under what circumstances family presence should end. The Palliative Care Network of Wisconsin provides an excellent template that facilities can adapt to their specific context.
Identify a core group of trained facilitators — ideally with representation from social work, chaplaincy, and experienced nursing staff. Training should cover the evidence base for FPDR, facilitator communication skills, family assessment, medical terminology translation, and the practical logistics of managing family presence during resuscitation. Ongoing refresher training should be incorporated into annual education cycles.
Resuscitation team members need to understand the evidence, know the facility protocol, and practice their roles in simulation scenarios that include family presence. Education should address common concerns — performance anxiety, litigation fears, family trauma — with evidence-based responses. A well-educated team is more likely to engage with FPDR constructively rather than reactively.
Building FPDR into your mock code program is one of the most practical investments a facility can make. Teams that have rehearsed FPDR scenarios handle real events with far greater confidence and professionalism.
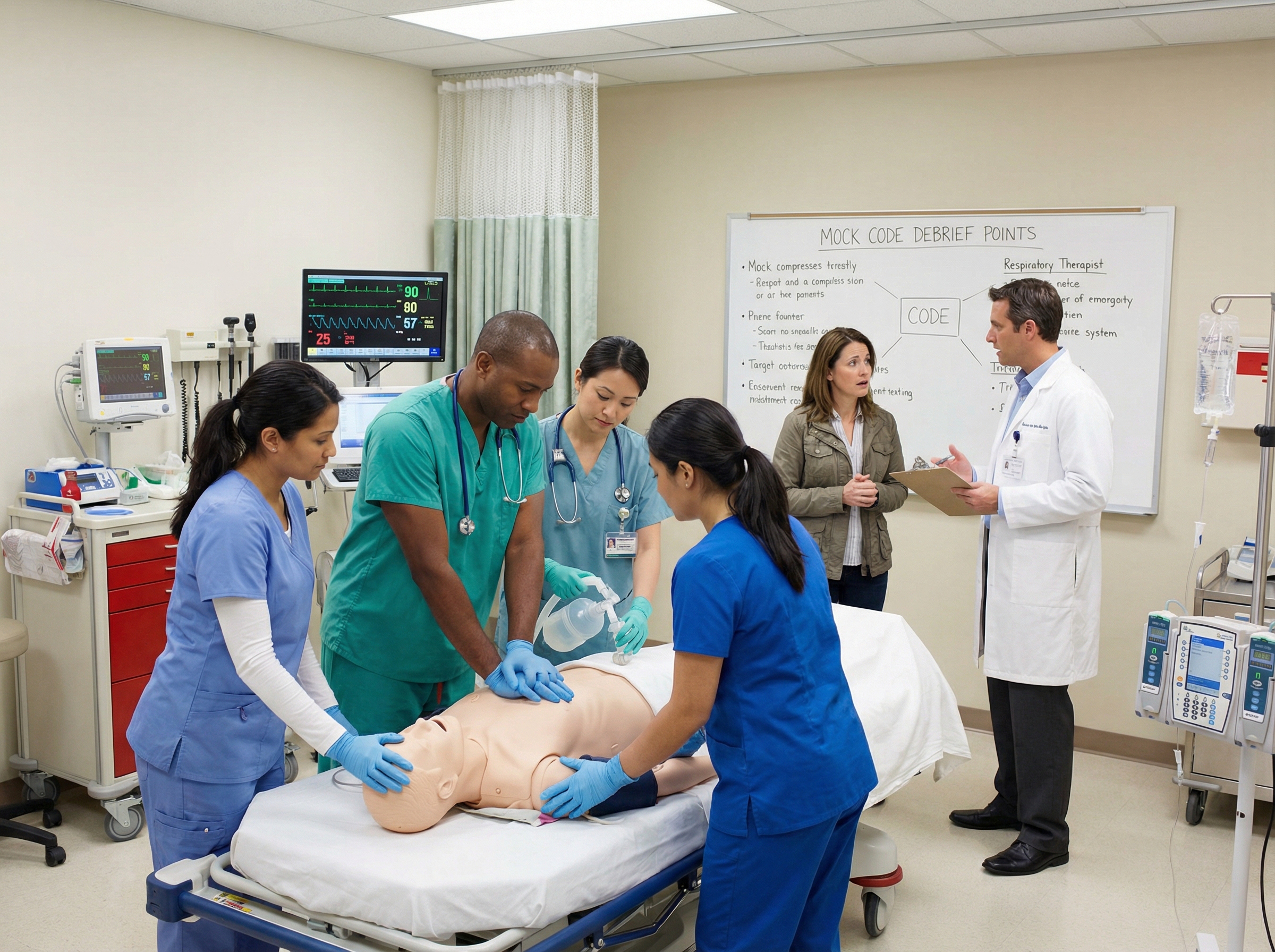
Debriefing is essential after any resuscitation event — and this is even more true when family members were present. Post-event debriefs allow the team to process what happened, identify what worked and what did not, and continuously refine the program. The role of debriefing after ACLS events extends beyond clinical performance — it also addresses the emotional and ethical dimensions of events where family presence added complexity. Facilitators should also debrief separately to process their own experience supporting grieving families.
Family presence during resuscitation is not a culturally neutral practice. Across different cultural traditions, the meaning of death, the role of family in end-of-life care, and expectations for family participation in medical events vary enormously. What is comforting in one cultural context may feel inappropriate or even alarming in another.
Healthcare teams that incorporate cultural competence in ACLS training are better equipped to navigate these conversations in real time. The facilitator plays a critical role here — assessing not only the family's emotional state but also their cultural framework for the event they are witnessing. When possible, integrating cultural or religious support resources into the FPDR process strengthens the program's responsiveness.
Ethically, FPDR sits at the intersection of several core principles: patient autonomy, family-centered care, and beneficence. While the patient may not be in a position to consent during an active resuscitation, prior expressed wishes — documented advance directives, POLST forms, or family conversations — should inform how FPDR decisions are made. When no prior preferences are known, offering FPDR as an option (not a requirement) respects family agency without creating pressure.
It is important to acknowledge that FPDR affects providers as well as families. Performing resuscitation while being observed by a grieving family introduces an additional emotional and psychological dimension to an already demanding clinical event. This is real, and it deserves acknowledgment.
Resuscitation events carry significant psychological weight for the clinicians who perform them. Adding family presence — particularly in cases involving children, young adults, or circumstances that mirror the provider's own life — can amplify that weight considerably. This is why grief support for medical professionals must be considered as an integrated part of any FPDR program, not an afterthought.
Institutions that implement FPDR without simultaneously investing in provider emotional support are setting their teams up for compounded stress and burnout. Peer support programs, access to counseling, and structured post-event debriefs are not luxuries — they are operational necessities for sustainable, compassionate practice.
Understanding how witnesses are affected by trauma applies not only to family members watching resuscitation but to providers performing it under observation. Creating a culture where providers can name and process these experiences without stigma is foundational to team resilience.
For newer clinicians and those who are early in their code team experience, FPDR can feel especially daunting. The combination of executing resuscitation skills correctly while managing awareness of a watching family is a significant cognitive and emotional load.
The most important thing new code team members can do is to focus on their defined role and trust the structure of the team. When everyone knows their assignment — and that assignment has been rehearsed — the presence of family becomes manageable. Building confidence as a new code team member is about repetition, role clarity, and developing trust in your team — all of which translate directly to performing well under FPDR conditions.
Seek out simulation opportunities that include FPDR scenarios. Ask experienced colleagues about their approaches to managing family presence. Read the evidence. The more informed and rehearsed you are before your first real FPDR event, the more effectively you will serve both the patient and the family in the room.
Navigating complex clinical and interpersonal scenarios like FPDR begins with a strong ACLS foundation. When your resuscitation algorithms, medication knowledge, and team communication skills are solid, you have far more cognitive bandwidth to manage the human dimensions of a code — including family presence.
At Affordable ACLS, our online ACLS certification course is developed by board-certified emergency medicine physicians with over 20 years of clinical experience. The course covers cardiac arrest algorithms, team dynamics, medications, and post-arrest care — all at your own pace, with unlimited retakes and immediate digital certification upon completion. ACLS certification starts at just $99, with recertification available for $89.
The better prepared you are in the clinical fundamentals, the more confidently you can show up for your patients — and their families — in the most difficult moments.
Family presence during resuscitation is not a trend or a policy debate — it is an evidence-based practice that, when implemented well, benefits families, supports patients, and strengthens the professional culture of resuscitation teams. The research is clear: FPDR does not compromise clinical quality, and it offers measurable psychological benefits for families facing the worst moments of their lives.
The path to effective FPDR runs through preparation: written protocols, trained facilitators, simulation-based team training, and a culture of open debriefing and provider support. None of this happens overnight, but every element is within reach for any healthcare team committed to family-centered care.
As an ACLS-certified provider, you are already equipped with many of the skills that make FPDR successful — algorithmic competence, team communication, situational awareness, and clinical composure under pressure. Adding the knowledge and preparation specific to family presence rounds out your ability to lead with both clinical excellence and compassion when it matters most.
.jpg)

