Organ transplantation is one of medicine's most extraordinary achievements, giving patients with end-stage organ failure a second chance at life. But behind every successful transplant lies a series of high-stakes clinical moments where cardiac emergencies can arise without warning — in the donor suite, the operating room, the ICU, and throughout the recipient's long recovery. For every professional on a transplant team, from transplant surgeons and anesthesiologists to procurement coordinators and critical care nurses, a firm command of Advanced Cardiovascular Life Support principles is not optional. It is a clinical imperative.
According to the Health Resources and Services Administration's organ donation statistics, more than 103,000 people are currently waiting for a lifesaving organ transplant, and 13 people die every day because a suitable organ does not arrive in time. With donation after circulatory death (DCD) heart transplant utilization rising by 77.7% between 2022 and 2023 alone, transplant teams are encountering more cardiac complexity than ever before. The clinicians who manage these patients need ACLS proficiency that goes well beyond the standard algorithm — they need to understand how resuscitation decisions directly affect organ viability, recipient outcomes, and ethical obligations.

This article walks through the specific cardiac emergency scenarios transplant teams face, the ACLS frameworks that apply, unique physiological considerations for both donors and recipients, team dynamics that save lives in the transplant setting, and how staying current on certification keeps every provider ready when seconds count.
Managing a brain-dead donor who develops hemodynamic instability or cardiac arrest is among the most clinically demanding scenarios in transplant medicine. The primary goal shifts from survival of the individual to preservation of viable organs for waiting recipients — yet the resuscitation interventions themselves must be evidence-based and executed with precision.
Brain death triggers a cascade of pathophysiological changes that profoundly destabilize cardiac function. Autonomic storms during herniation produce massive catecholamine surges followed by vasomotor collapse, resulting in profound hypotension, arrhythmias, and myocardial stunning. Diabetes insipidus causes rapid fluid shifts, while hypothyroidism, hypothermia, and coagulopathy compound the hemodynamic picture. Transplant ICU teams must anticipate and proactively address each of these derangements using ACLS-based frameworks adapted to the donor context.
The ACLS approach to reversible causes of cardiac arrest — commonly taught as the Hs and Ts framework — is especially relevant during donor management. Hypovolemia, hypoxia, hypothermia, hypo/hyperkalemia, hydrogen ion excess, tension pneumothorax, tamponade, toxins, and thrombosis — virtually every item on this checklist can manifest during donor care, particularly in the setting of prolonged ICU stays, aggressive resuscitation fluids, and neurogenic dysfunction.
Electrolyte disturbances deserve particular attention. Hyperkalemia-induced cardiac arrest is a recognized risk in organ donors, especially following massive blood transfusions, cell lysis from tissue damage, or renal insufficiency in the dying patient. Peaked T waves, widened QRS complexes, and sine wave patterns on ECG should trigger immediate treatment with calcium gluconate, sodium bicarbonate, insulin-dextrose, and if warranted, kayexalate or dialysis — all while maintaining organ perfusion pressure.
Donation after circulatory death (DCD) represents the intersection of resuscitation medicine and organ procurement in its most ethically nuanced form. In controlled DCD, life-sustaining therapy is withdrawn in a planned manner, and the surgical team assembles in anticipation. Once circulatory arrest is declared — following a mandatory hands-off interval of two to five minutes without resuscitation — procurement proceeds rapidly to minimize warm ischemic time.
What makes DCD scenarios so demanding for transplant clinicians is the deliberate cessation of resuscitative efforts and the strict time windows that govern organ viability. According to the American Heart Association and ILCOR scientific statement on organ donation after out-of-hospital cardiac arrest, potential organ donors were identified in 20% of patients managed with extracorporeal CPR versus 6% of those managed with conventional CPR — a finding that is reshaping how advanced resuscitation technologies are integrated into donation pathways.
Transplant teams must understand the boundary between resuscitation for survival and resuscitation for organ preservation. Once a patient transitions to a DCD pathway, standard ACLS interventions designed to restore the patient's own circulation are no longer appropriate. Instead, normothermic regional perfusion (NRP) and extracorporeal membrane oxygenation (ECMO) are increasingly used to perfuse the abdomen and thorax after circulatory death has been declared, preserving organ function without violating the dead donor rule. Familiarity with these technologies — and with the ACLS pharmacology that supports hemodynamic optimization before withdrawal — is essential for any clinician involved in DCD care.
DCD heart transplantation in particular has seen dramatic growth. A review of DCD heart transplant outcomes published in Circulation: Heart Failure documents how utilization has risen sharply over the past several years, driven by improved perfusion techniques and growing acceptance of DCD hearts as viable grafts. This growth places transplant teams at greater frequency of encounter with the unique resuscitation and preservation decisions that DCD pathways require.
If donor management is demanding, managing cardiac arrest in a transplant recipient is arguably more complex. Transplant recipients carry extraordinary physiological burdens: immunosuppressant-induced cardiomyopathy, drug interactions that alter arrhythmia thresholds, baseline renal or hepatic dysfunction that changes medication kinetics, and an immune system deliberately suppressed to prevent rejection. When a recipient arrests, the ACLS provider must adapt standard algorithms to this altered physiology at speed.
Heart transplant recipients present a particularly instructive case. According to the International Society for Heart and Lung Transplantation (ISHLT) guidelines for the care of heart transplant recipients, the denervated transplanted heart does not respond to atropine in the setting of bradycardia, since vagal tone has been surgically interrupted. An ACLS provider unaware of this fact who administers atropine for post-transplant bradycardia will get no response — the correct intervention is chronotropic agents such as isoproterenol or temporary pacing. This is a high-stakes knowledge gap that ACLS training specific to transplant settings must address.
Perioperative hemodynamic instability in the immediate post-transplant period can result from graft reperfusion injury, post-bypass inflammatory response, elevated pulmonary vascular resistance, and labile fluid status. Each of these requires a different ACLS-informed approach. Right ventricular failure following lung transplant, for example, demands aggressive optimization of pulmonary vascular resistance with inhaled nitric oxide or prostacyclin, volume management, and vasopressor support — all within the ACLS framework of systematic assessment and targeted intervention.
When a transplant recipient does arrest, the standard adult cardiac arrest circular algorithm remains the backbone of management. High-quality CPR, defibrillation for shockable rhythms, and systematic identification of reversible causes all apply. However, the reversible causes list takes on new dimensions in this population: acute rejection, calcineurin inhibitor toxicity causing QT prolongation and torsades de pointes, opportunistic infection triggering septic shock, and cardiac allograft vasculopathy (CAV) causing silent myocardial infarction are all on the differential.
Standard ACLS medications — epinephrine, amiodarone, lidocaine, adenosine — all remain relevant in the transplant population, but their use requires careful consideration of the transplant-specific context. Immunosuppressants such as tacrolimus and cyclosporine are metabolized via CYP3A4, and amiodarone is a potent CYP3A4 inhibitor. Co-administration can dramatically increase calcineurin inhibitor levels, leading to nephrotoxicity and neurotoxicity. While this does not preclude amiodarone use in a cardiac arrest — the immediate risk of death outweighs pharmacokinetic concerns — it does mandate close monitoring and dose adjustment in the post-resuscitation period.
The ACLS medications cheat sheet covering dosages, routes, and indications provides a rapid reference for providers during codes, but transplant teams benefit from supplementing this with a transplant-specific pharmacology overlay that addresses drug interactions, altered clearance in transplant recipients, and the hemodynamic effects of immunosuppression. Tacrolimus, for example, can prolong the QT interval and lower the threshold for ventricular arrhythmias — a fact that becomes critical when evaluating tachyarrhythmias in a post-transplant patient.
Vasopressor selection in the transplant recipient also warrants nuance. The evidence on epinephrine versus vasopressin in cardiac arrest is directly applicable here, but transplant teams also frequently use vasopressin infusions in both donor management and recipient stabilization because of its role in correcting the vasoplegia associated with brain death and post-bypass inflammatory states. Understanding the hemodynamic targets and titration principles behind vasopressor use equips transplant providers to make faster, better decisions at the bedside.
Transplant resuscitation events involve more personnel from more disciplines than almost any other code scenario in medicine. A cardiac arrest during organ procurement may simultaneously involve the transplant surgical team, procurement coordinators, anesthesia, perfusionists, critical care nurses, and organ preservation specialists. Without deliberate team structure and clear communication protocols, these events can become chaotic despite the presence of highly trained individuals.
The ACLS framework for closed-loop communication, defined roles, and a clear team leader is not merely theoretical in this context — it is the difference between an organized response and a fragmented one. Reviewing ACLS team dynamics and communication scripts is particularly valuable for transplant teams who may rarely perform resuscitations together but need to function seamlessly when they do.
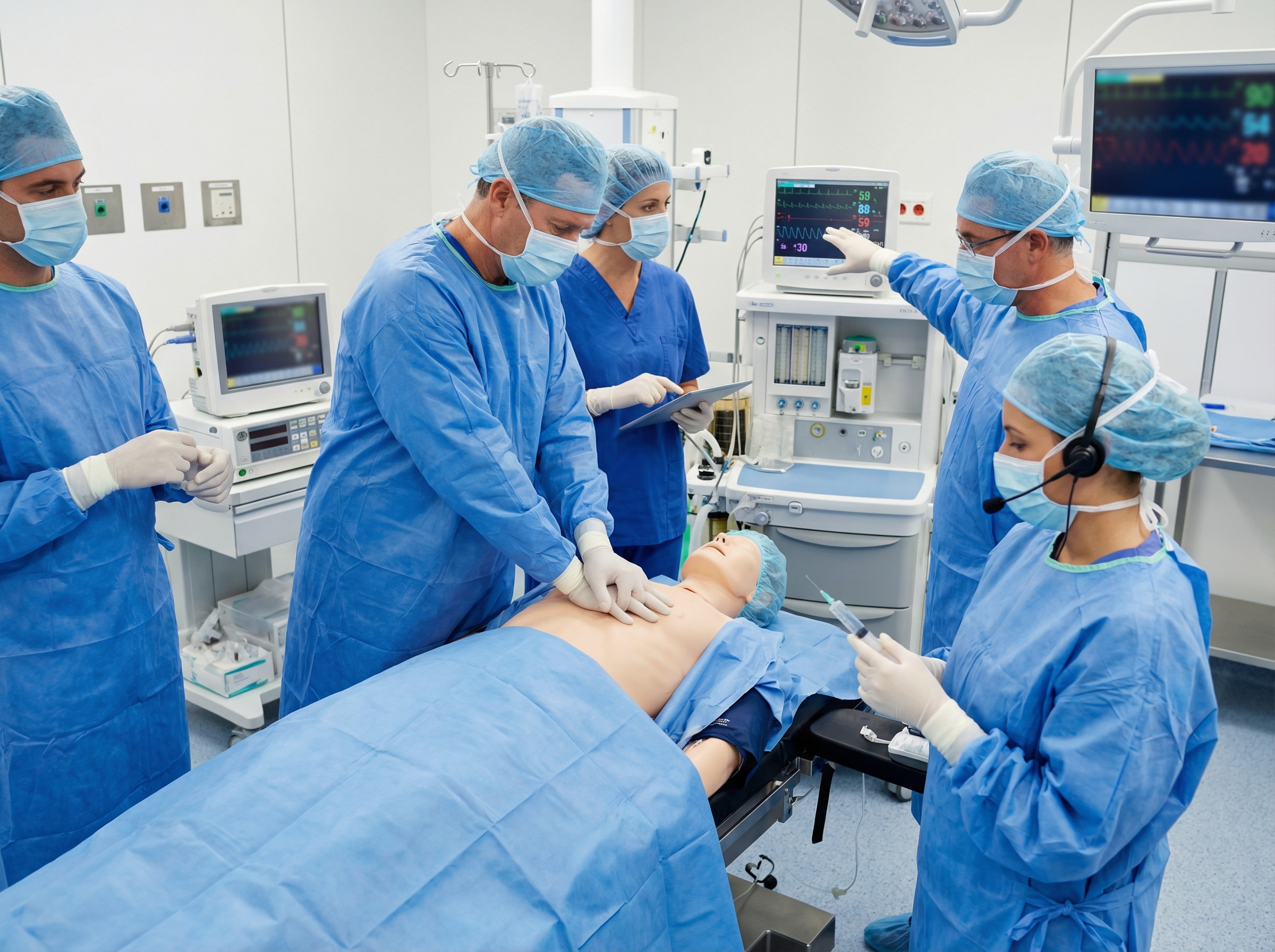
Role clarity is especially important in the transplant OR, where the surgical team's attention may be divided between the resuscitation effort and maintaining the sterility and viability of organs already procured. Designating a resuscitation team leader who is separate from the operative surgeon, assigning a dedicated pharmacist or nurse for medication preparation, and establishing clear communication channels between the code team and the organ preservation team are all practices that experienced transplant programs embed in their emergency protocols.
Simulation-based training that replicates transplant-specific arrest scenarios — including donor hemodynamic collapse, intraoperative arrest during procurement, and post-transplant arrest in the ICU — allows teams to rehearse these coordination challenges in low-stakes environments. Programs that invest in regular high-fidelity simulation alongside current ACLS certification consistently report faster response times and fewer critical errors during actual events.
When return of spontaneous circulation is achieved in a transplant recipient, the post-resuscitation period demands a systematic approach that accounts for the transplant-specific physiological baseline. The immediate post-cardiac arrest care algorithm guides providers through oxygenation and ventilation optimization, hemodynamic stabilization, targeted temperature management, coronary angiography consideration, and neurological prognostication — all of which require modification for the transplant population.
Targeted temperature management (TTM) in transplant recipients presents particular challenges. Immunosuppressant metabolism is temperature-dependent, and therapeutic hypothermia can increase drug exposure unpredictably. Graft function may also be affected by systemic cooling. Current evidence supports individualized temperature management decisions in transplant recipients, with close collaboration between the resuscitation team, transplant pharmacist, and transplant physician.
Hemodynamic optimization following ROSC in this population must address not only the standard goals of mean arterial pressure greater than 65 mmHg and adequate cardiac output, but also the specific perfusion requirements of the transplanted organ. A transplanted kidney, for example, may have limited autoregulatory reserve, making blood pressure targets higher than those used in the general post-arrest population. A transplanted liver is particularly sensitive to hypoperfusion in the early post-transplant period. These nuances require the resuscitation team to communicate closely with the transplant service during and after every code event. Research published in PMC's review of perioperative care for organ transplant recipients highlights that the paradigm of post-arrest care in this setting demands transplant-specific protocols that go well beyond standard guidelines.
Beyond the core frameworks, several specific cardiac emergency scenarios recur in transplant medicine and merit dedicated preparation.
Primary graft dysfunction (PGD) is the leading cause of early mortality after heart transplantation, occurring in approximately 25-30% of cases to some degree. Severe PGD manifests as profound cardiogenic shock within 24 hours of transplantation and can progress to cardiac arrest if not aggressively managed. ACLS providers caring for immediate post-heart-transplant patients must recognize PGD early — rising lactate, falling mixed venous oxygen saturation, worsening hemodynamics despite escalating vasopressor support — and escalate promptly to mechanical circulatory support, including intra-aortic balloon pump, Impella, or ECMO, before arrest occurs. When arrest does occur in this setting, the resuscitation must proceed with simultaneous activation of the ECMO team.
Acute cellular or antibody-mediated rejection can present with rapid hemodynamic deterioration, malignant arrhythmias, and cardiac arrest, particularly in the first year post-transplant. The ACLS approach to arrest is standard, but the post-ROSC evaluation must include urgent endomyocardial biopsy and echocardiography to assess rejection-related dysfunction. Recognizing rejection as a reversible cause — analogous to the Hs and Ts framework — is a cognitive habit that improves outcomes in this population.
Cardiac allograft vasculopathy (CAV) is a form of accelerated coronary artery disease that affects the transplanted heart and is a major cause of late graft failure. Because the transplanted heart is denervated, recipients do not experience typical angina and may present directly with ventricular arrhythmia or arrest as the first manifestation of significant CAV. This underscores the importance of annual surveillance angiography and the ACLS team's awareness that cardiac arrest in a heart transplant recipient beyond the first post-transplant year warrants immediate consideration of CAV-related ischemia as the precipitating cause.
Given the complexity of cardiac emergencies in the transplant setting, it is striking how often certification maintenance falls behind in this specialty. Transplant surgeons, coordinators, and critical care nurses frequently cite time constraints and scheduling difficulties as barriers to keeping ACLS current. Yet the cost of lapsed certification — in clinical preparedness, institutional liability, and ultimately patient outcomes — far exceeds the investment required to maintain it.
This is exactly the problem that Affordable ACLS was designed to solve. Founded by actively practicing, Board Certified Emergency Medicine physicians, Affordable ACLS delivers a 100% online, self-paced ACLS certification that busy transplant professionals can complete in one to two hours — at a cost of $99 for initial certification and $89 for recertification. The course is built on current AHA and ILCOR guidelines, includes unlimited retakes, provides immediate digital certification upon completion, and is backed by a money-back guarantee.
For transplant programs looking to keep entire teams compliance-ready, group certification solutions for healthcare facilities make it straightforward to manage multiple providers across departments. Whether a transplant coordinator needs to renew during a busy procurement season or a new surgical fellow needs initial ACLS certification before their first on-call shift, the flexibility of online certification removes the scheduling barriers that delay compliance in traditional in-person formats.
Transplant medicine's demands evolve constantly, and so do the guidelines that govern resuscitation practice. ACLS certification is not a one-time credential — it is a regular commitment to staying current with the evidence base that underpins every code response. For a specialty where a misstep during cardiac arrest can cost both a patient's life and the viability of organs that could save others, that commitment is foundational.
Beyond clinical preparedness, transplant programs are subject to regulatory scrutiny from the Organ Procurement and Transplantation Network (OPTN) and The Joint Commission, both of which have specific requirements around staff competency in emergency response. The HRSA has directed the OPTN to develop policies to better safeguard DCD patients and improve family communication throughout the donation process. Transplant programs that can demonstrate systematic ACLS certification maintenance and transplant-specific emergency protocols are better positioned in regulatory reviews.
Documentation of resuscitation events — including precise timing of interventions, medications administered, rhythm at each defibrillation, and post-ROSC vital signs — is equally critical in the transplant setting. This documentation supports quality improvement, informs protocol refinement, and provides the evidentiary record that transplant programs need when reviewing adverse outcomes. ACLS training that emphasizes documentation habits as part of the team leader role produces providers who capture this information even under pressure.
Organ transplantation saves lives — but only when every link in the chain of care holds under pressure. From the moment a donor's hemodynamics begin to destabilize to the late post-transplant ICU admission of a recipient presenting with arrhythmia, ACLS-trained professionals make the decisions that determine whether transplanted organs reach their recipients and whether recipients survive to use them.
Building a culture of resuscitation readiness in transplant medicine means more than checking a certification box. It means understanding the transplant-specific physiology that modifies every standard algorithm, staying current with the evolving evidence base on DCD, primary graft dysfunction, and post-transplant arrhythmia management, and practicing team-based resuscitation so that multi-disciplinary groups function cohesively when a real code occurs.
For transplant professionals ready to strengthen their ACLS foundation or bring their certification current, Affordable ACLS provides the most convenient, clinically credible, and cost-effective pathway available — built by ER physicians who understand exactly what it means to be the last line of defense for a critically ill patient. Visit www.affordableacls.com to get certified or recertified today, and make sure your transplant team is ready for every cardiac emergency that comes your way.
.jpg)

