The cardiac catheterization laboratory is one of the most technically demanding environments in modern medicine. Designed for precision, it houses some of the most advanced imaging and interventional technology available. But when a patient decompensates on the table, the cath lab transforms instantly into a resuscitation suite, and every team member must be ready to execute Advanced Cardiovascular Life Support with the same precision they apply to balloon catheters and stents.
For interventional cardiologists, nurses, radiologic technologists, and cath lab support staff, ACLS competency is not merely a credentialing requirement. It is a clinical lifeline. According to StatPearls research on cardiac catheterization risks, major complications including cardiac arrest, coronary perforation, and severe hemodynamic collapse occur in fewer than 3% of elective interventional procedures, yet in high-acuity settings such as primary PCI for STEMI, the stakes are considerably higher. Knowing exactly what to do in those critical minutes is the difference between a successful outcome and a tragedy.
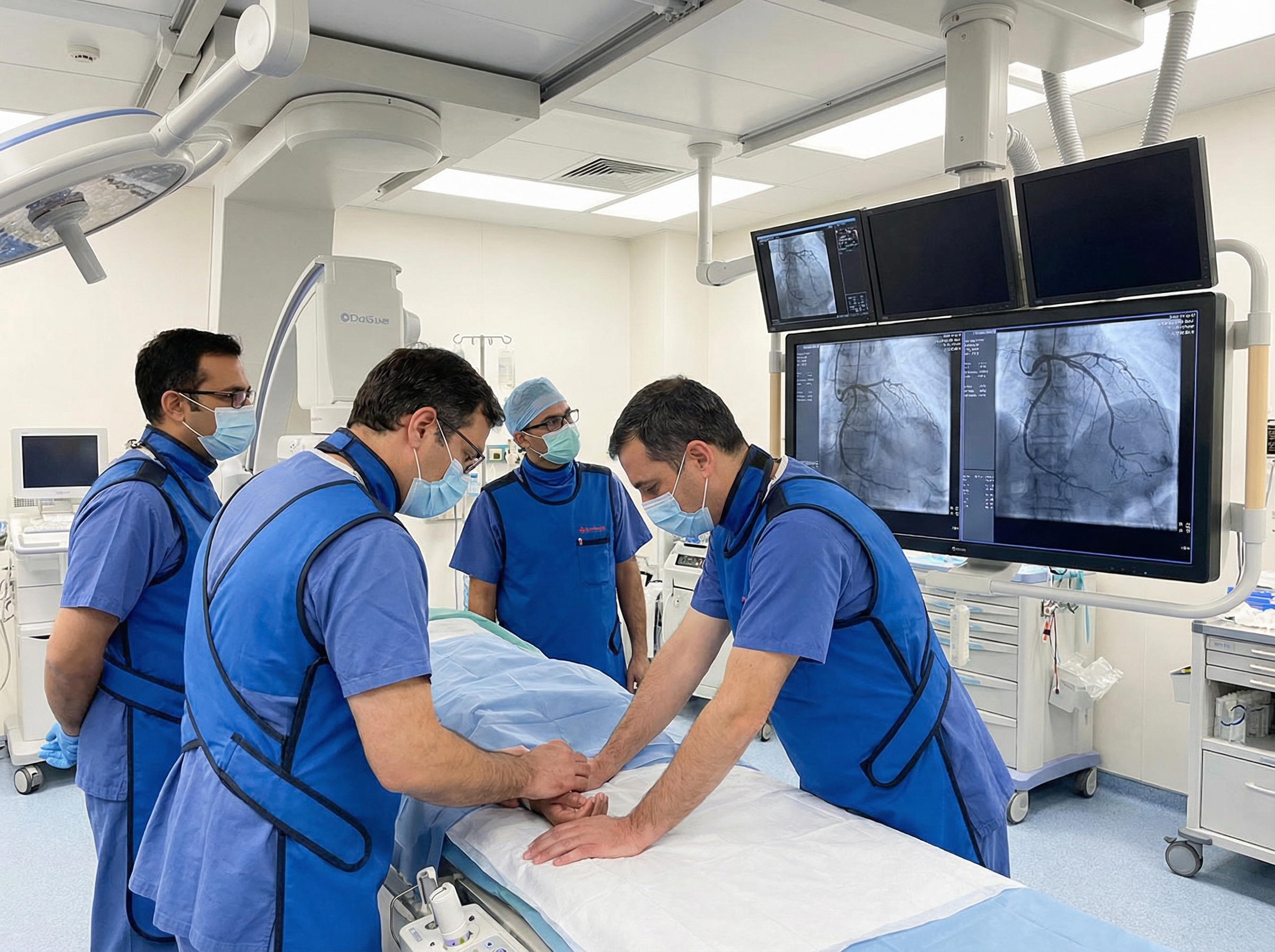
This article explores the specific ACLS challenges unique to the cardiac catheterization environment, the most common life-threatening complications encountered during interventional procedures, and the protocols that high-performing cath lab teams use to manage them effectively. Whether you are a seasoned interventionalist refreshing your knowledge or a cath lab nurse preparing for certification, this guide will sharpen your clinical edge.
Resuscitation in the cath lab differs from a standard code blue in important ways. The environment is physically constrained, with imaging equipment, sterile fields, and lead shielding limiting movement. The patient is often anticoagulated, adding hemorrhagic risk to any intervention. Radiation exposure protocols affect how quickly personnel can reposition. And critically, the precipitating cause of cardiac arrest is frequently identifiable and potentially reversible on the same table where resuscitation is occurring.
These factors create a resuscitation paradigm that differs meaningfully from standard ACLS. Cath lab teams must integrate conventional resuscitation algorithms with procedure-specific interventions, including the ability to continue or complete coronary intervention while compressions are underway. This requires not only ACLS competency but also a team dynamic built around clear role assignment, closed-loop communication, and pre-established protocols for the most likely scenarios.
Understanding how ACLS principles apply in this specialized setting begins with mastering the foundational algorithms. Cath lab professionals who complete or refresh their knowledge of the key changes in ACLS guidelines for 2025 will be better equipped to translate those updates into cath lab-specific practice.
Several life-threatening events are disproportionately common in the cath lab environment. Each carries a distinct clinical signature, a specific ACLS response, and nuances that every team member should internalize.
Ventricular fibrillation (VF) is the most feared arrhythmia in the cath lab and also the most treatable when recognized immediately. Myocardial irritation from guidewires, balloon inflations, or contrast injections can provoke VF at any point during the procedure. In acute STEMI patients undergoing primary PCI, the ischemic myocardium is already electrically unstable, making spontaneous VF a constant threat.
When VF is detected on the monitor, the response must be instantaneous. Defibrillation is the definitive treatment, and every second of delay reduces survival probability by approximately 7 to 10 percent. The defibrillator in a properly equipped cath lab should always be charged and ready. Staff must ensure pads are correctly placed, confirm all personnel are clear, and deliver the shock without waiting. High-quality CPR begins immediately following the shock and continues until a rhythm check reveals return of organized activity.
For a thorough review of the rhythms most commonly encountered in this setting, the resource on shockable rhythms including ventricular tachycardia and fibrillation provides essential background that every cath lab clinician should master.
Coronary perforation is a rare but potentially catastrophic complication of PCI, with an incidence of approximately 0.5 percent. However, according to research published in Circulation: Cardiovascular Interventions, perforation is associated with a 13-fold increase in major adverse cardiovascular events and a fivefold increase in 30-day mortality, underscoring how quickly this complication can become lethal.
Blood escaping into the pericardial space causes cardiac tamponade, a clinical emergency characterized by the Beck triad of hypotension, jugular venous distension, and muffled heart sounds. In the cath lab, tamponade can develop rapidly and must be recognized before the patient loses blood pressure entirely. Bedside echocardiography, increasingly available in modern cath labs, is invaluable for confirming pericardial effusion.
The ACLS approach to tamponade centers on immediate pericardiocentesis to relieve pressure on the heart. Volume resuscitation and vasopressors provide temporary hemodynamic support, but drainage is the only definitive intervention. Cath lab teams should be familiar with the clinical presentation and management pathway described in the comprehensive overview of pericardial effusion and cardiac tamponade.
Right coronary artery (RCA) interventions carry a specific risk of inducing bradycardia and even complete heart block due to the RCA's role in supplying the sinoatrial and atrioventricular nodes in most patients. Contrast injection into the RCA, balloon occlusion, or reperfusion can all trigger a vasovagal response or direct nodal injury resulting in profound bradycardia.
Cath lab protocols for RCA procedures typically include having atropine drawn and ready at the bedside. For persistent, symptomatic bradycardia that does not respond to atropine, transcutaneous pacing via the defibrillator pads provides a bridge while transvenous pacing is arranged. Staff must be proficient with pacing mode activation on the cath lab defibrillator and understand the indications and technique.
The adult bradycardia with a pulse algorithm provides a structured decision framework that guides clinicians through the exact sequence of assessment and intervention steps appropriate to this scenario, and every cath lab team member should have it committed to memory.
Beyond VF, a range of tachyarrhythmias can destabilize a patient during interventional procedures. Sustained ventricular tachycardia (VT) with a pulse, rapid atrial fibrillation with hemodynamic compromise, and supraventricular tachycardias can all precipitate a hemodynamic crisis on the cath lab table. The underlying ischemic substrate in most cath lab patients makes these rhythms particularly dangerous.
The first determination is whether the patient is hemodynamically stable or unstable. An unstable patient, defined by hypotension, altered mental status, chest pain, or signs of acute pulmonary edema, requires immediate synchronized cardioversion. The ACLS protocol mandates sedation if the patient is conscious, followed by a synchronized shock at the recommended energy level. Cath lab teams who have reviewed the comprehensive guide to synchronized cardioversion will be able to execute this sequence rapidly and safely.
For patients who are relatively stable, the adult tachycardia with a pulse algorithm guides the approach through rhythm assessment and pharmacologic versus electrical therapy decisions. Adenosine, amiodarone, and beta-blockers each have distinct roles depending on the rhythm, and dosing accuracy is critical in the anticoagulated cath lab patient.
One of the most operationally complex scenarios in cath lab resuscitation is the need to continue or complete coronary intervention while the patient is in cardiac arrest and CPR is underway. Manual chest compressions interrupt fluoroscopic imaging, introduce radiation exposure risks for the compressor, and make fine catheter manipulation nearly impossible.
Mechanical chest compression devices represent a critical advance in this context. Devices such as the AutoPulse and LUCAS systems deliver continuous, consistent compressions that free the interventionalist's hands and allow uninterrupted fluoroscopy. According to the Society for Cardiovascular Angiography and Interventions guidance on managing cardiac arrest in the cath lab, mechanical compression devices improve the rate of return of spontaneous circulation and enable initiation of percutaneous circulatory support during active resuscitation.
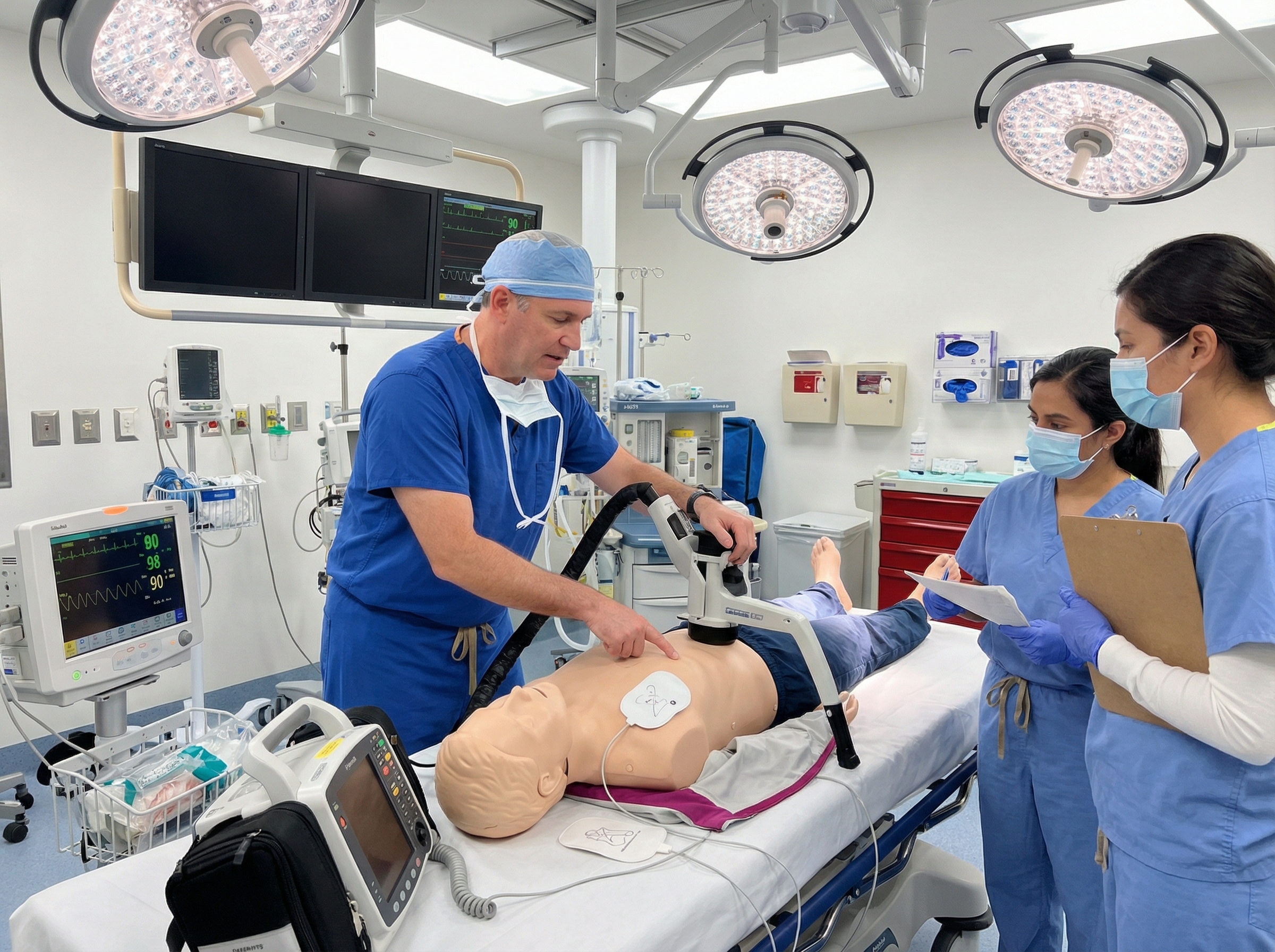
Cath labs that see high volumes of primary PCI for STEMI should have mechanical compression devices immediately accessible and all staff trained in their rapid deployment. The decision to continue PCI during CPR should be made by the team leader, weighing the likelihood that restoration of coronary flow is necessary for ROSC against the practical limitations of the specific case.
Cardiogenic shock complicating PCI represents a spectrum from mild hypotension responsive to vasopressors to refractory collapse requiring full mechanical circulatory support. The cath lab is increasingly the site where these decisions are made in real time, often before a formal ICU transfer is feasible.
According to the 2025 ACC Expert Consensus Statement on the Evaluation and Management of Cardiogenic Shock, early hemodynamic assessment within the first 12 hours is associated with significantly lower in-hospital mortality. Devices including intra-aortic balloon pumps (IABP), Impella devices, and extracorporeal membrane oxygenation (ECMO) are now deployed in high-volume centers with increasing frequency during high-risk PCI.
For cath lab clinicians, understanding the hemodynamic profile of cardiogenic shock, including reduced cardiac output, elevated filling pressures, and increased systemic vascular resistance, is essential for recognizing when additional support is needed and communicating that need clearly to the team. Vasopressors such as norepinephrine and dopamine provide temporary bridge support but do not address the underlying cause. The definitive intervention remains restoration of coronary perfusion.
Cath lab nurses and technologists should also understand the pharmacologic toolkit used in these scenarios. The ACLS medications cheat sheet covering dosages, routes, and indications is a practical reference that ensures every team member can anticipate, prepare, and administer the correct agents under pressure.
The cardiac cath lab is the definitive treatment setting for acute coronary syndrome, but ACS itself can evolve and complicate procedures in unexpected ways. Abrupt vessel closure, side branch occlusion, distal embolization of thrombus, and no-reflow phenomenon can all produce acute clinical deterioration that demands immediate ACLS-level response.
The no-reflow phenomenon, defined as inadequate myocardial perfusion despite a patent epicardial artery following PCI, produces chest pain, ST elevation or depression, and hemodynamic instability that can be misinterpreted as a new complication or equipment failure. Recognition depends on correlating angiographic findings with clinical status. Treatment includes intracoronary vasodilators such as adenosine, verapamil, or nicardipine, and may require hemodynamic support if the affected territory is large.
Cath lab professionals who have internalized the acute coronary syndrome algorithm will be better prepared to recognize when a procedural complication is producing ACS-level hemodynamic crisis and communicate that clearly to the team leader. The pathophysiology of ischemia also directly informs ECG changes that the team must track throughout the procedure.
For a deeper understanding of the ECG changes that accompany myocardial ischemia and guide decision-making in the cath lab, the guide on ECG interpretation in myocardial ischemia is an invaluable resource for all cath lab personnel, not just physicians.
The defining feature of high-performing cath lab resuscitation teams is pre-assignment of roles before the case begins, not after the monitor alarmed. In a standard ACLS code, role assignment happens at the time of the arrest. In the cath lab, the team is already assembled around the table. The risk, however, is that role confusion in this unique environment delays critical interventions.
Best practice calls for a brief pre-procedure checklist that includes identification of the team member responsible for defibrillation, who will initiate compressions, who manages the airway, and who communicates with pharmacy and the broader care team. In STEMI cases or high-risk PCI, this review should be standard. Research supports that structured team communication significantly reduces response time and error rates during resuscitation events.
The physiologic complexity of cath lab arrests, including anticoagulation, vascular sheaths, active contrast administration, and ongoing fluoroscopy, makes closed-loop communication even more important than in standard resuscitation environments. Confirmation of every order, read-back of every drug dose, and explicit acknowledgment of every intervention reduces the chance of error in a noisy, high-pressure setting.
Cath lab resuscitation demands immediate access to a specific set of ACLS medications, as well as cath lab-specific pharmacology that overlaps with resuscitation. Epinephrine remains the cornerstone vasopressor in cardiac arrest, administered at 1 mg IV every 3 to 5 minutes. Amiodarone at 300 mg IV is the first-line antiarrhythmic for shock-refractory VF and pulseless VT, with a second dose of 150 mg available if needed.
Beyond standard ACLS medications, the cath lab formulary typically includes heparin, bivalirudin, glycoprotein IIb/IIIa inhibitors, vasopressors, intracoronary vasodilators, and reversal agents. Staff must know not only what these medications do but how they interact with the resuscitation context. For example, reversal of anticoagulation may be necessary to address coronary perforation and tamponade, but premature reversal risks stent thrombosis in a freshly deployed stent.
According to a systematic review of intra-procedural arrhythmias during cardiac catheterization, atropine and adenosine are among the most commonly deployed emergency medications during catheterization procedures, and pre-drawn syringes at the field during high-risk cases can reduce administration time by critical seconds. Every cath lab should conduct regular drills that include medication preparation and administration sequences.
When ROSC is achieved in the cath lab, the team's work is far from finished. Post-cardiac arrest care begins immediately at the point of resuscitation and includes optimization of hemodynamics, ventilatory management, and targeted temperature management when appropriate. The cath lab team must stabilize the patient sufficiently to complete the necessary interventional procedure if it has not already been done, then facilitate safe transfer to the cardiac intensive care unit.
According to a narrative review of PCI post out-of-hospital cardiac arrest, there is strong evidence that immediate coronary angiography and PCI improve survival with good neurological outcomes in patients resuscitated from cardiac arrest with ST elevation. This means that in many cases, completing the PCI is itself a post-resuscitation intervention, and the cath lab team must be prepared to continue working after ROSC in a patient who remains critically ill.
Hemodynamic targets in the post-arrest period include a mean arterial pressure of at least 65 mmHg, avoidance of hypoxia and hyperoxia, and glucose management. Vasopressors such as norepinephrine are first-line for persistent hypotension. Mechanical circulatory support should be considered early if vasopressors alone are insufficient. Communication with the receiving ICU team must be structured, clear, and include a full account of the arrest event, the interventions performed, and the current clinical status.
Understanding the STEMI activation pathway is fundamental to cath lab emergency preparedness. The interval from first medical contact to balloon inflation, or door-to-balloon time, is a direct predictor of myocardial salvage and survival. When activation is delayed or miscommunicated, the patient arrives in a more compromised state, increasing the probability of in-lab cardiac arrest.
The detailed breakdown of cardiac cath lab activation for subtle acute inferior STEMI illustrates how seemingly ambiguous ECG presentations can evolve rapidly into life-threatening situations requiring immediate cath lab mobilization. Cath lab team members who understand these nuances are better prepared to respond to patients who arrive in an unstable condition or deteriorate on the table.
Similarly, understanding the full interventional pathway described in the resource on percutaneous coronary intervention as a lifeline for acute coronary syndrome helps contextualize why in-lab complications occur and what physiologic processes are at stake during every PCI procedure.
ACLS certification is required for most cardiac catheterization laboratory positions, and for good reason. The clinical scenarios described throughout this article demand not just theoretical knowledge but practiced, automatic execution of life-saving algorithms under extreme pressure. Certification ensures that all team members share a common framework, use consistent terminology, and can collaborate seamlessly when every second matters.
For cath lab professionals who need to earn or renew their ACLS certification, Affordable ACLS offers a 100% online, self-paced program developed by Board Certified Emergency Medicine physicians. The course is AHA and ILCOR compliant, covers all the core algorithms relevant to cath lab practice, and provides immediate certification upon completion. With unlimited retakes and a money-back guarantee, it is a practical, accessible option for busy cath lab staff.
The course content directly addresses the cardiac arrest algorithms, hemodynamically unstable arrhythmia management, post-cardiac arrest care, and medication protocols that form the backbone of cath lab emergency response. At just $99, with discounts available for group enrollment, it delivers genuine clinical value at a fraction of the cost of in-person options.
The cardiac catheterization laboratory demands the highest level of clinical preparedness from every team member. Life-threatening complications can occur without warning, in patients who are already critically ill, in a physical environment that creates unique resuscitation challenges. ACLS is not a background credential for cath lab professionals. It is an active, continuously practiced clinical skill set that directly influences patient outcomes.
From ventricular fibrillation management to coronary perforation response, from mechanical circulatory support to post-arrest care, the principles of ACLS run through every emergency protocol in the interventional suite. Teams that invest in certification, simulation-based training, and pre-procedure role assignment will perform better when the monitor alarms and there is no time to think through the next step.
If you are a cath lab professional looking to earn or renew your ACLS certification, Affordable ACLS is designed for clinicians like you. Built by emergency medicine physicians, delivered entirely online, and compliant with the latest guidelines, it provides the clinical depth and the credential you need. Visit www.affordableacls.com or call 866-655-2157 to get started today.
.jpg)

