Cardiac arrest remains one of the most time-sensitive emergencies in medicine. Every second of delay in identifying the underlying cause reduces the chance of meaningful survival. For decades, Advanced Cardiovascular Life Support (ACLS) teams have relied on clinical assessment, rhythm analysis, and algorithmic reasoning to guide resuscitation. But a powerful tool has been reshaping how skilled clinicians manage these critical moments: point-of-care ultrasound, or POCUS.
POCUS refers to bedside ultrasound performed and interpreted in real time by the treating clinician, rather than a radiologist. In the setting of cardiac arrest, this portable imaging technology allows providers to visualize the heart, identify reversible causes, assess cardiac activity, and guide critical interventions—all while the resuscitation continues. As the evidence base grows and equipment becomes more accessible, POCUS is no longer a niche skill reserved for academic medical centers. It is becoming an expected competency in emergency and critical care environments nationwide.
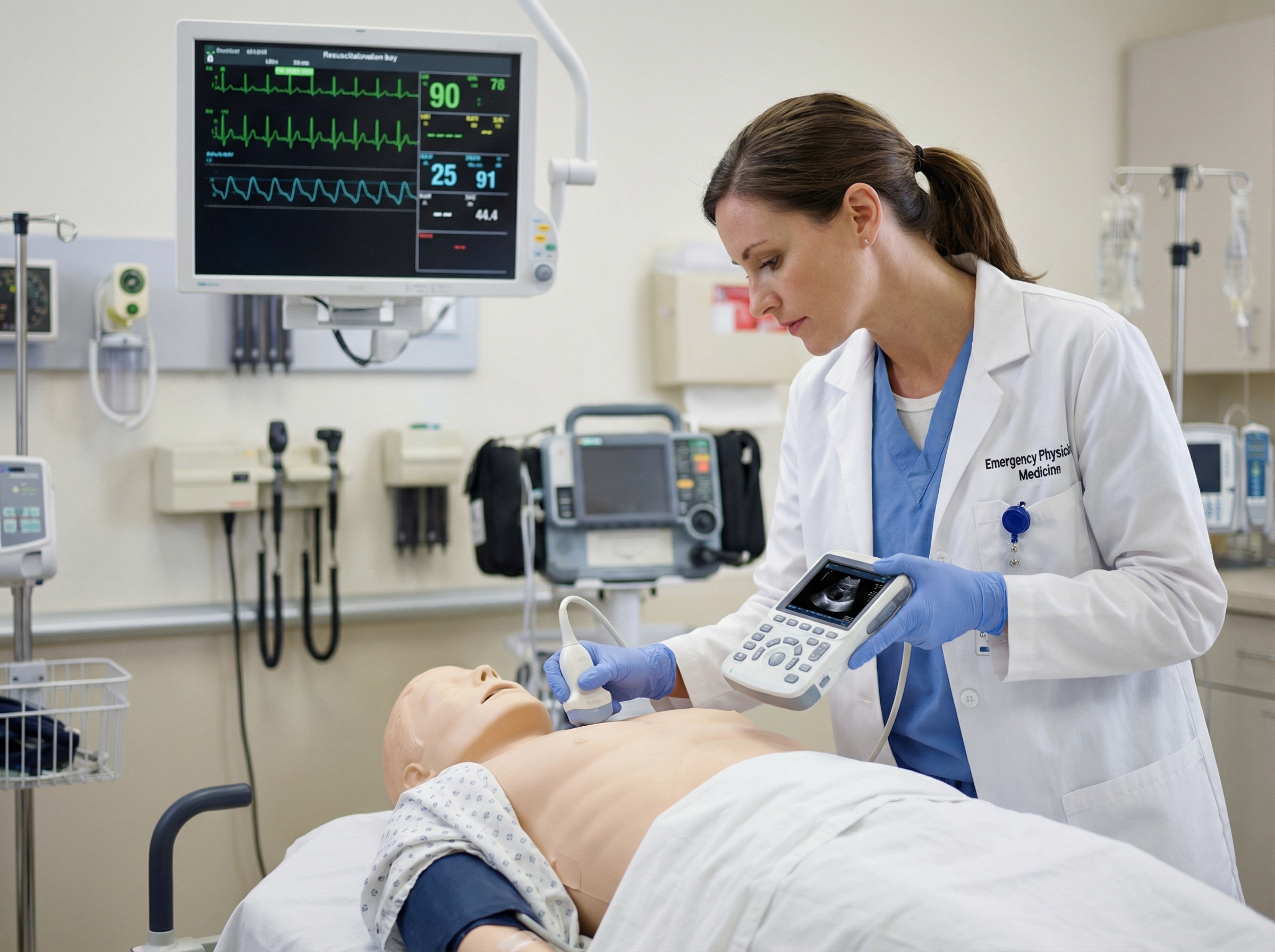
This article explores how POCUS is integrating into ACLS practice, what the 2025 American Heart Association guidelines say about its use, and what every clinician involved in resuscitation needs to know about applying it safely and effectively.
Point-of-care ultrasound is a focused, goal-directed imaging examination performed at the bedside for a specific clinical question. Unlike comprehensive echocardiography conducted by a cardiologist or sonographer, POCUS during cardiac arrest is designed to answer narrow but critical questions quickly: Is there cardiac motion? Is there a pericardial effusion? Is the right ventricle severely dilated? Is there evidence of tension pneumothorax or massive pulmonary embolism?
Cardiac arrest is predominantly a non-shockable rhythm problem. Pulseless electrical activity (PEA) and asystole together account for the majority of in-hospital cardiac arrests, with research indicating these non-shockable rhythms represent approximately 81% of cases in the United States. The challenge with PEA, in particular, is that the electrical system appears to be functioning while the mechanical pump has failed—often because of a reversible underlying cause. Standard ACLS assessment tools alone may miss these causes. POCUS offers a direct window into the thoracic cavity to find them.
A 2025 comparative study found that POCUS identified reversible causes in 72.5% of cardiac arrest cases, compared to just 42.5% with standard ACLS assessment alone. The sensitivity of POCUS in identifying these causes was 87.5%, versus 56.5% for standard ACLS approaches. These are not marginal gains. They represent a substantial improvement in the clinician's ability to find and treat what is killing the patient.
The foundation of ACLS resuscitation is the systematic search for reversible causes, summarized in the classic mnemonic of the Hs and Ts. Several of these causes are directly identifiable—or at least strongly suggested—by POCUS during active resuscitation.
Hypovolemia can be assessed by evaluating inferior vena cava (IVC) diameter and collapsibility. A flat, collapsible IVC in the setting of cardiac arrest strongly suggests volume depletion, guiding immediate fluid resuscitation. Cardiac tamponade, one of the most treatable causes of obstructive shock and cardiac arrest, is directly visualized as a pericardial effusion with associated right heart collapse. Without POCUS, tamponade can be nearly impossible to diagnose during active CPR using clinical examination alone. With POCUS, it is identified within seconds.
Tension pneumothorax can be identified by the absence of lung sliding and the presence of the stratosphere sign on M-mode, indicating air in the pleural space rather than normal lung movement. Massive pulmonary embolism causes acute right ventricular dilation, which can be visualized on the subcostal or parasternal cardiac views. When a clinician sees a markedly dilated, hypokinetic right ventricle during cardiac arrest, pulmonary embolism must be strongly considered as the etiology—and immediate intervention, including consideration of thrombolytics, becomes the priority.
Of all the reversible causes of cardiac arrest, cardiac tamponade is perhaps the one where POCUS has the most dramatic and immediate clinical impact. Pericardial effusion and cardiac tamponade occur when fluid accumulates in the pericardial sac, compressing the heart and preventing adequate filling. In the extreme case of cardiac arrest from tamponade, the diagnosis must be made rapidly and pericardiocentesis performed without delay.
The subcostal four-chamber view is typically the most accessible cardiac window during active CPR and allows the clinician to scan the pericardial space in under five seconds. The presence of an anechoic (dark) fluid collection surrounding the heart, combined with right atrial or right ventricular diastolic collapse, confirms tamponade physiology. This is information that cannot be obtained from a rhythm strip, blood pressure monitoring, or clinical examination alone during active resuscitation.
When tamponade is identified, the team can prepare for emergency pericardiocentesis while CPR continues—rather than discovering the diagnosis post-mortem. This is the precise scenario where POCUS saves lives that would otherwise be lost. According to a comprehensive clinical review in Diagnostics, bedside identification of tamponade during resuscitation represents one of the highest-yield applications of POCUS across all emergency medicine settings.
Massive pulmonary embolism causing cardiac arrest is another scenario where POCUS provides critical diagnostic information unavailable through other means. When a large clot obstructs the pulmonary vasculature, right ventricular afterload rises dramatically, causing the right ventricle to dilate acutely. In the context of cardiac arrest or peri-arrest state, this pattern of acute right heart strain on POCUS should immediately trigger consideration of pulmonary embolism as the primary etiology.
Understanding the relationship between shock and pulmonary embolism helps clinicians recognize that the right ventricular dilation seen on POCUS is not incidental—it is the anatomical consequence of sudden, massive obstruction. When combined with the clinical context of unexplained cardiac arrest, absence of other obvious causes, and prior history of immobility or hypercoagulability, a dilated right ventricle on POCUS justifies the significant decision to administer systemic thrombolytics during cardiac arrest.
Research from the Annals of Emergency Medicine indicates that integrating POCUS into cardiac arrest management protocols specifically addresses this diagnostic gap, allowing teams to make more informed decisions about thrombolysis in undifferentiated cardiac arrest when PE is suspected. The decision carries substantial risk, and POCUS-derived evidence of RV dilation meaningfully shifts the risk-benefit calculation in favor of treatment.
One of the most clinically important—and sometimes misunderstood—applications of POCUS in cardiac arrest is the assessment of cardiac mechanical activity. The ECG rhythm tells you about electrical conduction. POCUS tells you about mechanical response. These two pieces of information are not always concordant.
True asystole on the monitor can sometimes be accompanied by subtle cardiac mechanical activity on ultrasound—a phenomenon sometimes called pseudo-PEA or near-death cardiac activity. Conversely, an organized ECG rhythm in PEA can show a completely motionless heart on ultrasound, indicating a lower probability of achieving return of spontaneous circulation (ROSC). Studies have consistently demonstrated that the presence of cardiac motion on POCUS during PEA is associated with higher rates of ROSC and survival. This information guides the team's resuscitative intensity and, in some cases, the decision to continue or cease efforts.
Equally important is the detection of occult ventricular fibrillation. In approximately 3 to 5% of cardiac arrests, ventricular fibrillation is present but not detected on surface ECG due to fine amplitude, lead placement issues, or artifact. POCUS can reveal the characteristic chaotic mechanical activity of ventricular fibrillation even when the ECG appears flat or unclear. Detecting occult VF is critical because it is a shockable rhythm—one with significantly better outcomes than asystole when treated promptly with defibrillation. Missing this diagnosis means missing a potentially life-saving intervention.
The most significant concern about incorporating POCUS into active cardiac arrest management is the risk of interrupting chest compressions. High-quality, minimally interrupted CPR is the cornerstone of effective resuscitation. Any diagnostic tool that causes clinicians to pause compressions for extended periods ultimately harms the patient, regardless of the information gained. This is why the development of structured protocols for POCUS use during cardiac arrest has been critically important.
The Cardiac Arrest Sonographic Assessment (CASA) exam was developed specifically to address this concern. The protocol standardizes how POCUS is integrated into resuscitation without sacrificing CPR quality. Key elements include pre-positioning the ultrasound probe at the subcostal window before the pulse check begins, obtaining a brief image clip during the rhythm check—which should last no more than 10 seconds in total—and then resuming compressions immediately while the team reviews the captured clip. The sonographer does not hold compressions for image acquisition; the image is captured during the planned pause already built into the ACLS algorithm, then interpreted after CPR resumes.
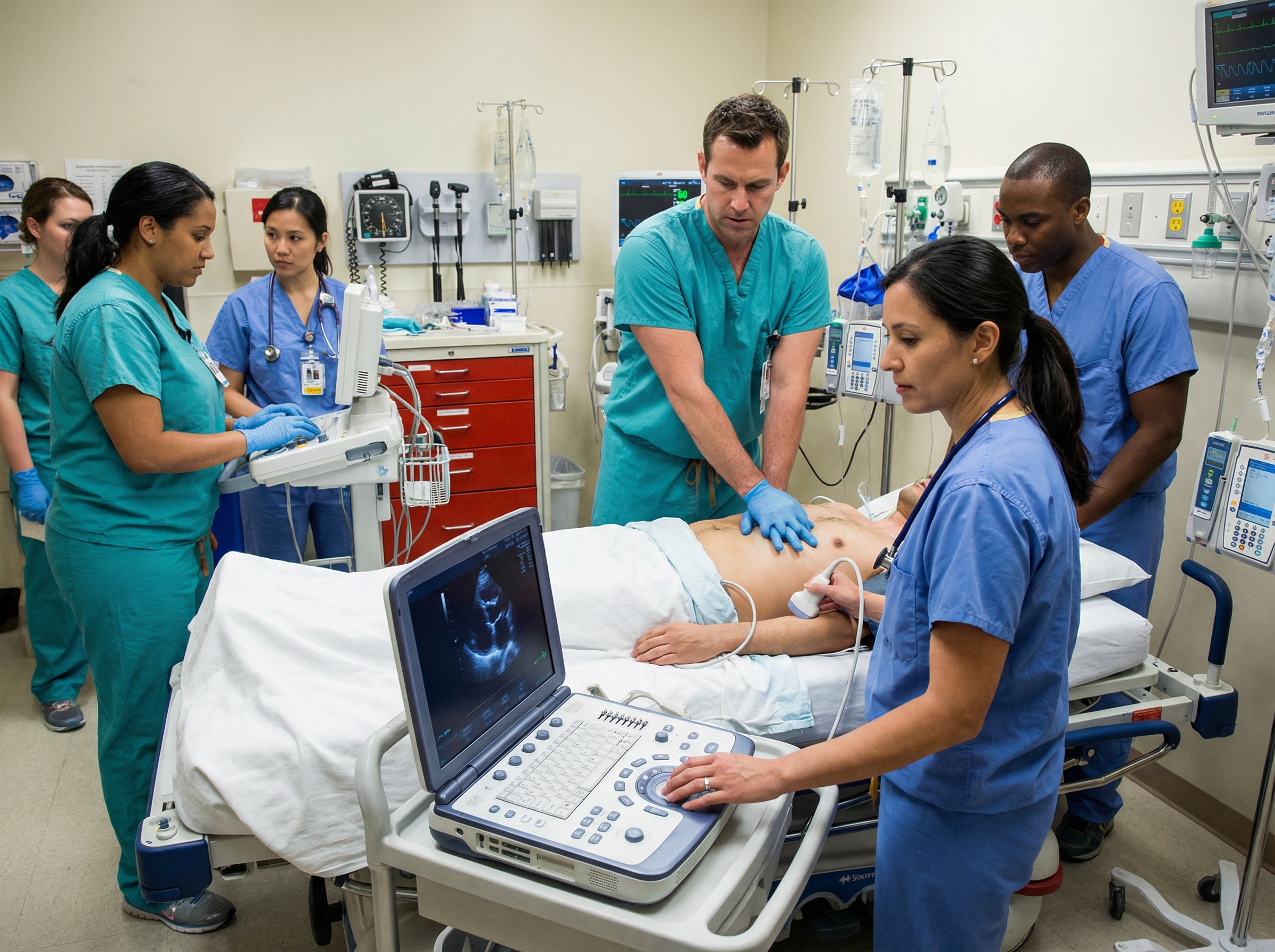
This approach allows POCUS to be integrated into the adult cardiac arrest algorithm without adding additional no-flow time. The most experienced sonographer available should be assigned the POCUS role, and the team leader must explicitly assign this role during the resuscitation rather than leaving it to chance. Role clarity and pre-assignment are essential for POCUS to enhance rather than disrupt resuscitation flow.
The 2025 American Heart Association guidelines for Adult Advanced Life Support address POCUS directly, representing a significant step in the formal integration of this technology into mainstream ACLS practice. According to the 2025 AHA ACLS Guidelines published in Circulation, the use of POCUS by experienced professionals during cardiac arrest may be considered to diagnose reversible causes, provided it does not interrupt resuscitative efforts. This is a notable evolution from prior guideline iterations, reflecting the growing body of evidence supporting POCUS utility in resuscitation.
The guidelines also acknowledge that POCUS for prognostication during cardiac arrest is not yet well established as a standalone tool. While cardiac mechanical activity on POCUS is associated with better outcomes, the absence of cardiac motion should not be used in isolation to terminate resuscitation efforts. This nuance is important: POCUS informs clinical decision-making but does not replace it. The decision to cease resuscitation must integrate the full clinical picture—duration of arrest, underlying cause, patient wishes, and the overall trajectory of the resuscitation effort.
For the clinician keeping pace with key changes in ACLS guidelines for 2025, understanding the POCUS recommendations is increasingly essential. The guidelines also support the post-ROSC use of echocardiography or point-of-care cardiac ultrasound to identify clinically significant diagnoses requiring intervention after return of spontaneous circulation is achieved.
The role of POCUS does not end when the patient achieves return of spontaneous circulation. In the immediate post-cardiac arrest care period, POCUS continues to provide valuable clinical information. A focused cardiac ultrasound after ROSC can rapidly assess left and right ventricular function, identify wall motion abnormalities suggesting acute myocardial infarction, evaluate volume status through IVC assessment, and confirm the absence of pericardial effusion that might have developed or worsened during resuscitation.
Post-ROSC cardiac dysfunction is common and can be severe. Myocardial stunning following prolonged ischemia can cause profound left ventricular dysfunction even in patients without underlying structural heart disease. POCUS allows the clinician to quickly characterize this dysfunction and guide hemodynamic support decisions—whether to initiate vasopressors, consider mechanical circulatory support, or request urgent cardiology consultation for possible catheterization.
The integration of POCUS into post-arrest care is aligned with AHA guideline recommendations supporting echocardiography as a reasonable post-ROSC assessment tool. A systematic review of POCUS imaging in cardiac arrest clinical outcomes found that POCUS provides meaningful diagnostic and prognostic information across multiple phases of cardiac arrest care, reinforcing its role both during active resuscitation and in the post-arrest period.
No clinical tool is without limitations, and POCUS is no exception. Several important limitations must be understood by any clinician incorporating POCUS into cardiac arrest management.
First and most critically: POCUS must never interrupt high-quality CPR. Research consistently demonstrates that no-flow time is a primary determinant of neurological outcome after cardiac arrest. An overly prolonged pause for image acquisition negates any diagnostic benefit. Clinicians without robust POCUS skills may struggle to obtain adequate images quickly under the pressure of active resuscitation, potentially causing more harm than benefit. This reinforces the need for dedicated training and clear role assignment before the team encounters an actual arrest.
Second, image quality in the resuscitation environment can be poor. Body habitus, subcutaneous emphysema, active chest compressions, and the chaotic physical environment of a code all degrade ultrasound image quality. The operator must be capable of recognizing when images are inadequate and avoid making critical decisions based on non-diagnostic studies.
Third, POCUS findings must always be interpreted in clinical context. The presence of cardiac motion does not guarantee ROSC; the absence of cardiac motion in an early arrest with a potentially reversible cause does not mandate termination. As noted in the 2025 AHA guidelines, POCUS informs but does not supplant clinical judgment. The decision to continue or discontinue resuscitation must integrate the complete clinical picture, including etiology, duration, patient factors, and the trajectory of the resuscitation effort.
Finally, not all hospitals and pre-hospital systems have the equipment or trained personnel to implement POCUS during cardiac arrest. This creates an equity gap in resuscitation quality that the medical community must continue to address through training investment, equipment availability, and protocol development.
For clinicians and resuscitation teams looking to meaningfully incorporate POCUS into their cardiac arrest management, the following practical considerations provide a framework for safe and effective implementation.
The trajectory of POCUS in ACLS is clearly toward broader adoption, deeper integration, and more sophisticated applications. Handheld ultrasound devices are now smaller and more affordable than ever, reducing the barrier to access in emergency departments, intensive care units, and even pre-hospital environments. Some EMS systems are beginning to explore POCUS use in the field, though protocols and evidence for this application continue to develop.
Artificial intelligence-assisted image interpretation is emerging as a potential tool to reduce the skill dependence of POCUS and improve reliability in the hands of less experienced operators. AI algorithms capable of automatically identifying pericardial effusion, RV dilation, and cardiac motion from ultrasound clips during resuscitation could substantially expand access to POCUS-guided resuscitation, though clinical validation of these tools is ongoing. The clinicians who remain at the cutting edge of technological innovations transforming ACLS training are best positioned to adopt these advances as they mature.
Serial POCUS assessment—using ultrasound at multiple time points during resuscitation rather than a single snapshot—is another area of active investigation. A 2025 study in the Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine explored serial POCUS during cardiac arrest to predict termination of resuscitation, reflecting growing interest in using dynamic ultrasound assessment to guide real-time decision-making throughout prolonged resuscitation efforts. Early findings suggest that trajectory of cardiac motion over time may provide more prognostic information than a single snapshot assessment.
For clinicians committed to excellence in resuscitation, understanding where the evidence is heading—and preparing their skills accordingly—is both a professional responsibility and a patient care imperative. POCUS in cardiac arrest is not a futuristic concept. It is current standard-of-care in leading emergency and critical care centers, and it is rapidly becoming expected practice everywhere else.
As tools like POCUS reshape resuscitation practice, staying current with ACLS certification is more important than ever. Affordable ACLS was founded by Board Certified Emergency Medicine physicians who understand both the clinical realities of cardiac arrest management and the time constraints clinicians face. Our 100% online, self-paced ACLS certification course covers cardiac arrest algorithms, reversible causes, team dynamics, advanced airways, defibrillation, and post-arrest care—all aligned with the latest AHA and ILCOR guidelines.
ACLS certification through Affordable ACLS is available for $99, with renewal pricing at $89. Certification is immediate upon successful completion, and unlimited retakes are included at no additional cost. Whether you are renewing your existing certification or obtaining ACLS for the first time, our physician-developed content prepares you for the complexities of real resuscitation—including the growing role of POCUS in guiding clinical decisions at the bedside.
The clinician who walks into a code confident in their algorithms, their team communication skills, and their ability to integrate emerging tools like POCUS is the clinician who gives their patient the best possible chance. Visit affordableacls.com or contact us at 866-655-2157 to get started with your ACLS certification today.
.jpg)

