In the fast-moving world of emergency medicine, seconds are not just precious — they are the difference between life and death. Cardiac arrest, severe arrhythmias, and life-threatening rhythm disturbances demand instant, accurate identification and decisive action. For decades, clinicians have relied on hard-won expertise, high-fidelity training, and established protocols like Advanced Cardiovascular Life Support to navigate these critical moments. Now, artificial intelligence is entering that same high-stakes arena, offering tools that can analyze electrocardiographic data with remarkable speed and precision, and increasingly guide resuscitation teams toward optimal decisions.

This transformation is not a distant promise. Research published in 2025 by the European Heart Rhythm Association, the Heart Rhythm Society, and the ESC Working Group on E-Cardiology confirms that AI has reached a level of clinical maturity in cardiac electrophysiology that demands serious attention from every healthcare professional. Understanding how these technologies work, what they can and cannot do, and how they interact with the ACLS protocols you already know is now essential professional literacy for emergency medicine practitioners. For a deeper foundation on where this journey began, explore the impact of AI on emergency cardiac care and see how the trajectory has accelerated in recent years.
The electrocardiogram has been the cornerstone of cardiac rhythm assessment since Willem Einthoven pioneered the technology in the early twentieth century. Human interpretation of the 12-lead ECG requires years of training, a thorough understanding of electrophysiology, and an ability to recognize subtle pattern deviations under pressure. Artificial intelligence approaches this challenge differently — and in many ways, more efficiently.
Modern AI-driven ECG analysis systems employ deep neural networks and convolutional architectures trained on millions of labeled ECG recordings. Rather than applying a set of manually coded rules, these models learn to recognize the statistical signatures of each arrhythmia class directly from data. The results have been striking. According to a comprehensive review published in PMC, deep learning models have achieved accuracy rates ranging from 79.4% to 99.93% for arrhythmia classification, with F1 scores approaching 100% for major arrhythmia categories on benchmark databases. A separate study highlighted accuracy of 99.43% using the MIT-BIH database, setting a high bar for clinical-grade automated interpretation.
What makes this especially valuable in an ACLS context is that these models operate in real time. An AI system embedded in a monitoring device or hospital information system can flag a potentially shockable rhythm, identify ST-segment changes consistent with acute ischemia, or recognize the onset of ventricular fibrillation before a human eye has finished scanning the strip. For anyone building the ECG interpretation skills that underpin effective ACLS response, a thorough review of ECG interpretation in myocardial ischemia provides the clinical grounding needed to work alongside these AI tools effectively.
Among the highest-stakes decisions in resuscitation is whether to deliver a defibrillatory shock. Ventricular fibrillation and pulseless ventricular tachycardia are the two shockable rhythms in the ACLS cardiac arrest algorithm, and early defibrillation is the single intervention most consistently associated with improved survival. Any technology that accelerates or improves the accuracy of that identification has profound life-saving potential.
Automated External Defibrillators already incorporate rudimentary shock-advisory algorithms, but these are being rapidly enhanced by machine learning. A 2025 study introduced what researchers called "Frugal AI" — a deep learning system capable of real-time shockable rhythm detection using a single-lead ECG and minimal computing hardware, making it deployable even in resource-constrained environments. More sophisticated hospital-grade systems use combined convolutional neural network and LSTM (Long Short-Term Memory) architectures to distinguish VF from non-shockable rhythms with exceptional sensitivity, even in the presence of motion artifact and CPR compression interference, which has historically been one of the most vexing technical challenges in automated rhythm analysis.
For clinicians who want to reinforce their own understanding of when and why to shock, the foundational concepts are covered in detail in understanding shockable rhythms including ventricular tachycardia and fibrillation. The better a provider understands the underlying physiology, the better equipped they are to verify, complement, and act on AI-generated rhythm assessments.
Atrial fibrillation is the most commonly encountered significant arrhythmia in clinical practice, affecting tens of millions of people worldwide and carrying substantial risk of stroke, heart failure, and hemodynamic compromise. Early detection is critical, yet AF is notoriously variable in its presentation and can be missed even by experienced practitioners, particularly in paroxysmal or silent forms.
AI has demonstrated particular strength in this domain. Deep neural networks trained on 12-lead ECGs have achieved sensitivities and specificities in the 90% to 99% range for AF classification. More remarkably, research reviewed in the Journal of Medical Internet Research demonstrated that an AI-ECG model could predict new-onset atrial fibrillation from sinus rhythm recordings with an AUC of 0.87 — outperforming the established CHARGE-AF clinical risk score (AUC 0.78). In other words, the AI found patterns predictive of future AF in ECGs that looked normal to the human eye.
This predictive capability is a meaningful shift in the clinical paradigm. Rather than simply confirming a rhythm already visible on the monitor, AI systems may soon alert providers to patients who are about to deteriorate — enabling pre-emptive intervention and richer ACLS decision-making. Combined with wearable monitoring technologies that provide continuous ECG data streams, the scope for early detection and timely escalation is expanding dramatically. To understand the clinical management landscape into which these AI tools are being introduced, reviewing the causes, symptoms, and treatments of atrial fibrillation remains as important as ever.
Beyond rhythm recognition, artificial intelligence is beginning to function as a real-time decision support partner during resuscitation. The ACLS algorithms — the systematic flowcharts for cardiac arrest, bradycardia, tachycardia, and post-cardiac arrest care — were designed to impose structure on a chaotic environment. AI-driven clinical decision support systems take that structure further by ingesting multi-variable patient data and generating prioritized recommendations during an active resuscitation.
Research from the University of Gothenburg produced SCARS-1, a machine learning system trained on 393 patient and event variables to predict 30-day survival probability after cardiac arrest. This kind of tool can inform real-time decisions about the aggressiveness and duration of resuscitation efforts — a profoundly difficult call that clinicians currently make based on experience and incomplete information. A complementary line of research published in the Journal of Medical Internet Research evaluated ChatGPT-4's performance in cardiac arrest and bradycardia simulations using AHA ACLS guidelines, finding that large language models can already engage meaningfully with ACLS case scenarios — a preview of how conversational AI might serve as a cognitive aid during high-pressure events.
The key caveat, clearly stated in multiple systematic reviews, is that while AI applications in resuscitation demonstrate encouraging performance, clear evidence of improved patient outcomes in routine clinical practice remains an ongoing area of investigation. The majority of published studies have been retrospective, and the field awaits large prospective trials. This makes provider education and protocol mastery not less important, but more important — because AI tools still require informed human oversight to be deployed safely and effectively. Keeping current with the key changes in ACLS guidelines for 2025 ensures providers understand the evolving clinical context within which these AI systems are being validated.
One of the persistent challenges in deploying AI in high-stakes clinical environments is the black box problem. Deep neural networks can produce extraordinarily accurate outputs while offering little transparency about why they reached a particular conclusion. For a cardiologist or emergency physician, accepting a diagnosis without understanding the reasoning behind it creates both clinical and medicolegal discomfort.
The field of Explainable AI (XAI) is directly addressing this challenge. Techniques such as SHAP (SHapley Additive exPlanations), Grad-CAM, and attention mechanisms produce visual or quantitative explanations that highlight which features of an ECG most influenced a model's classification. As reported in Frontiers in Cardiovascular Medicine, the ECG-XPLAIM model represents a locally adaptive architecture specifically designed to provide clinically interpretable explanations alongside its arrhythmia detection outputs. Similarly, research in npj Digital Medicine demonstrated deep learning ensembles using genetic programming approaches that generate interpretable arrhythmia detection outputs, bringing the field closer to tools that clinicians can trust, interrogate, and incorporate into their reasoning.
For healthcare teams, this development means that AI-generated rhythm assessments will increasingly come with supporting rationale — heatmaps over ECG traces, probability scores, and flagged intervals — rather than bare verdicts. This human-AI collaborative model is widely considered the most appropriate and safest framework for clinical deployment, and it closely mirrors the deliberate, team-based approach that ACLS training cultivates in every certified provider.
The integration of AI with consumer and clinical wearable devices represents one of the most rapidly advancing frontiers in cardiac care. Smartwatches equipped with single-lead ECG capabilities can now flag atrial fibrillation episodes for millions of users who would otherwise be unaware of intermittent rhythm disturbances. More advanced clinical wearables provide continuous multi-lead monitoring with AI analysis running in the cloud, capable of detecting not only AF but ventricular ectopy, bradyarrhythmias, and early signs of ischemia.
The clinical significance of this shift is enormous. Paroxysmal arrhythmias that previously escaped detection during brief office-based ECGs or Holter monitoring windows can now be captured during normal daily activities. A scoping review published in PMC specifically examined AI-driven rhythm detection in athletes — a population at elevated risk for concealed structural heart disease and lethal arrhythmias — finding promising accuracy for continuous monitoring applications. As these data streams feed into clinical records, the challenge becomes intelligently triaging AI-generated alerts to distinguish clinically significant findings from noise, a skill that requires strong foundational knowledge of rhythm interpretation and ACLS principles.
High-quality CPR is the foundation of successful resuscitation. Compression rate, depth, recoil, and minimization of interruptions are the controllable variables most strongly associated with return of spontaneous circulation. AI is now being applied to monitor and optimize these parameters in real time, providing feedback to resuscitating providers through smart CPR devices, accelerometer-equipped defibrillators, and audio-visual coaching systems.
According to a narrative review in PMC on AI in cardiopulmonary resuscitation, these real-time feedback systems have demonstrated improvements in compression quality metrics in both training and clinical settings. AI algorithms can also analyze the ECG during active compressions to assess rhythm without pausing CPR — a capability that directly improves the no-flow fraction and has been shown to enhance outcomes in experimental settings. This combination of feedback coaching and rhythm-during-compressions analysis represents a meaningful evolution in how resuscitation teams function in the field and in-hospital.
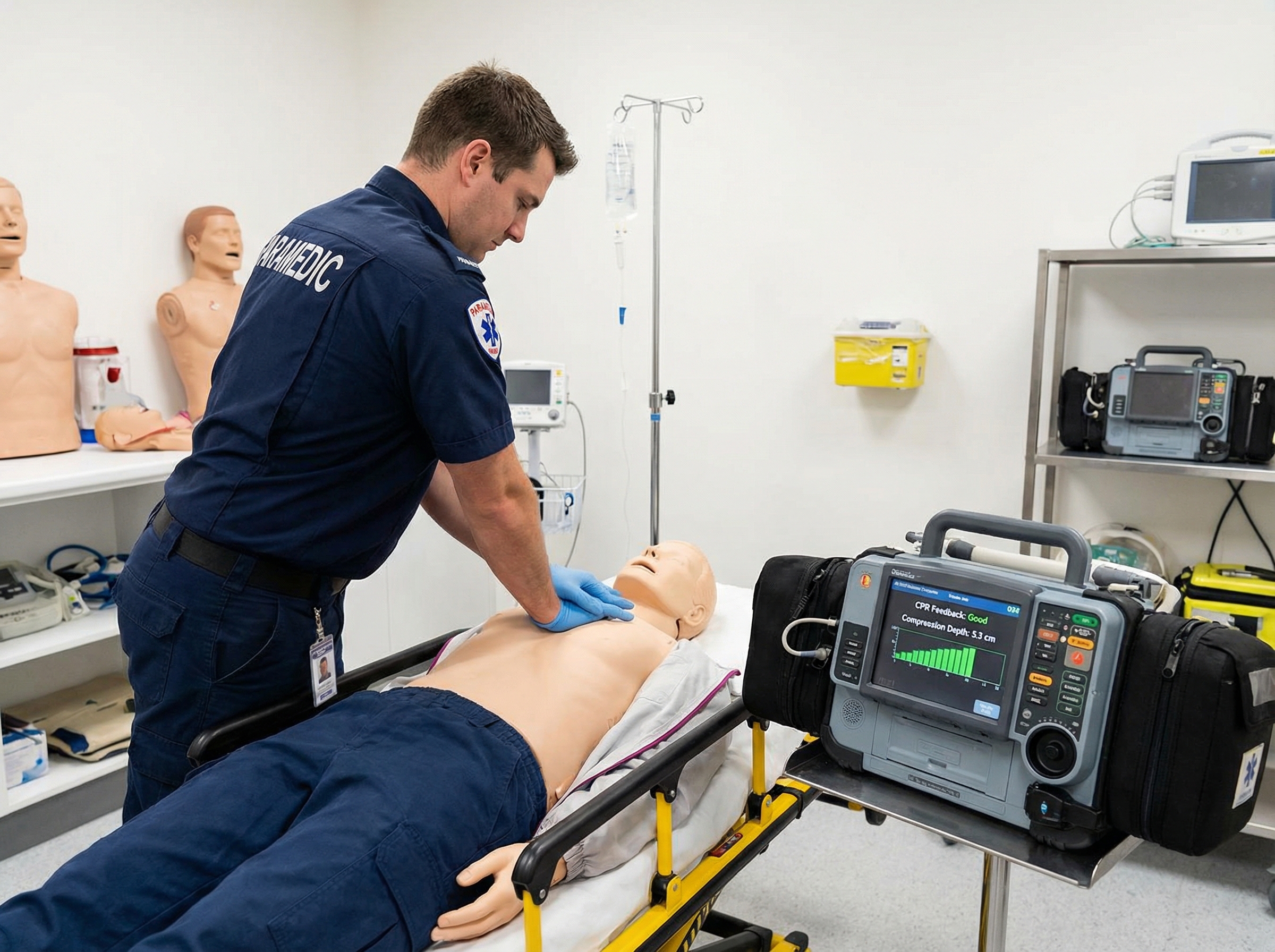
Understanding how AI amplifies the impact of well-trained providers — rather than replacing them — underscores why certification and skills-based training remain foundational. The evolution of these tools is also central to the top technological innovations transforming ACLS training, which explores how simulation, digital feedback, and AI-assisted learning environments are reshaping how providers prepare for cardiac emergencies.
The integration of artificial intelligence into cardiac care is still in its early chapters, but the pace of development is accelerating. Several convergent trends are shaping the near-term future. First, multimodal AI systems that combine ECG analysis with vital sign trends, laboratory values, imaging data, and patient history are under active development. These systems aim to provide a comprehensive clinical picture rather than a single-parameter rhythm call, bringing the AI assessment closer to the holistic judgment a seasoned emergency physician brings to a resuscitation.
Second, the regulatory and standardization landscape is maturing. Professional societies including the American Heart Association, the European Heart Rhythm Association, and the Heart Rhythm Society are actively developing frameworks for AI validation, clinical implementation standards, and integration into updated ACLS guidelines. The 2025 scientific statement from EHRA, HRS, and the ESC Working Group on E-Cardiology marks a significant milestone in this institutionalization process, providing a consensus framework for evaluating AI applications in clinical electrophysiology.
Third, AI-powered simulation and training environments are transforming how providers learn and practice ACLS skills. Adaptive learning platforms can identify knowledge gaps, customize scenario difficulty, and generate real-time performance feedback — compressing the learning curve and improving retention. These developments are already influencing the top trends shaping the future of ACLS in the next decade, making it clear that the relationship between AI and emergency cardiac care will only deepen in the years ahead.
The rapid advancement of AI in cardiac rhythm detection and ACLS decision support carries a direct message for every provider who holds or seeks ACLS certification: the baseline of clinical competence is rising. AI tools will become a standard feature of the clinical environment — embedded in monitors, defibrillators, EHR systems, and mobile devices. Providers who understand both the capabilities and the limitations of these systems will be able to leverage them as force multipliers. Those who do not risk being passive observers of AI outputs rather than active, critically informed clinicians.
This means that strong foundational training in ECG interpretation, arrhythmia recognition, and ACLS algorithms is not a substitute for AI — and AI is not a substitute for it. The two are genuinely complementary. AI raises the floor of rhythm detection performance across skill levels and reduces cognitive load during high-stress resuscitations. But it cannot replace the judgment, communication skills, team leadership, and ethical reasoning that define excellent emergency care. For providers exploring the broader landscape of digital tools supporting emergency practice, digital health and ACLS apps for emergency preparedness offers a practical overview of how technology and training intersect.
Staying current also means revisiting your certification and knowledge base regularly. ACLS guidelines evolve, AI applications are being incorporated into updated training standards, and the clinical evidence base is growing rapidly. Online certification platforms like Affordable ACLS provide AHA/ILCOR-compliant courses developed by Board Certified Emergency Medicine physicians — courses that integrate current clinical science with the flexible, self-paced format that fits the schedules of working healthcare professionals. ACLS certification is available at $99 (or $89 for recertification), with unlimited retakes and an immediate digital certificate upon completion, ensuring that the process of maintaining your credentials is as efficient as the AI tools now entering your clinical environment.
Artificial intelligence is not replacing the ACLS-trained provider. It is becoming the most sophisticated clinical collaborator that provider has ever had — one that never tires, processes information at extraordinary speed, and brings pattern recognition capabilities that exceed what any individual clinician can sustain across a long shift. Cardiac rhythm detection is being transformed by deep learning models with near-perfect accuracy on benchmark datasets, and ACLS decision support is being enhanced by systems that integrate dozens of variables to guide resuscitation strategy in real time.
But the technology is only as good as the team deploying it. AI-generated alerts still require interpretation. Shock advisory recommendations still require provider confirmation. Outcome prediction models still require human judgment about goals of care. The emergency physician, nurse, or paramedic who understands the physiology, knows the algorithms, and has practiced the skills under pressure remains the irreplaceable center of the cardiac arrest response.
Investing in your ACLS education — whether you are seeking initial certification or renewing your credentials — is an investment in your ability to work effectively in a clinical environment that AI is making more capable by the year. Explore what the latest advancements in cardiology mean for your practice, stay current with evolving guidelines, and approach AI as the powerful clinical tool it is — one that makes well-trained providers more effective, not obsolete. Visit Affordable ACLS to explore certification options built for today's healthcare professionals by physicians who understand both the science and the stakes.
.jpg)

