A routine tooth extraction. A straightforward crown preparation. A patient who arrived anxious and left in full cardiac arrest. For dental professionals who administer sedation, these scenarios are not hypothetical. They happen in private offices, oral surgery suites, and periodontal clinics every year, and the difference between a near-miss and a fatality often comes down to one question: is your team prepared to execute Advanced Cardiovascular Life Support protocols the moment things go wrong?
Dental sedation has transformed patient comfort and expanded the scope of outpatient oral care. Moderate conscious sedation, deep sedation, and general anesthesia now allow providers to complete complex cases on anxious, medically complex, or pediatric patients who would otherwise be impossible to treat. But every level of sedation carries cardiovascular and respiratory risk that no amount of pre-procedural screening eliminates entirely. As the American Dental Association notes, cardiovascular events, vasovagal syncope, allergic reactions, and airway compromise remain among the most frequently encountered medical emergencies in dental settings. For providers working beyond the BLS level, ACLS certification is not a box to check. It is a clinical survival skill.
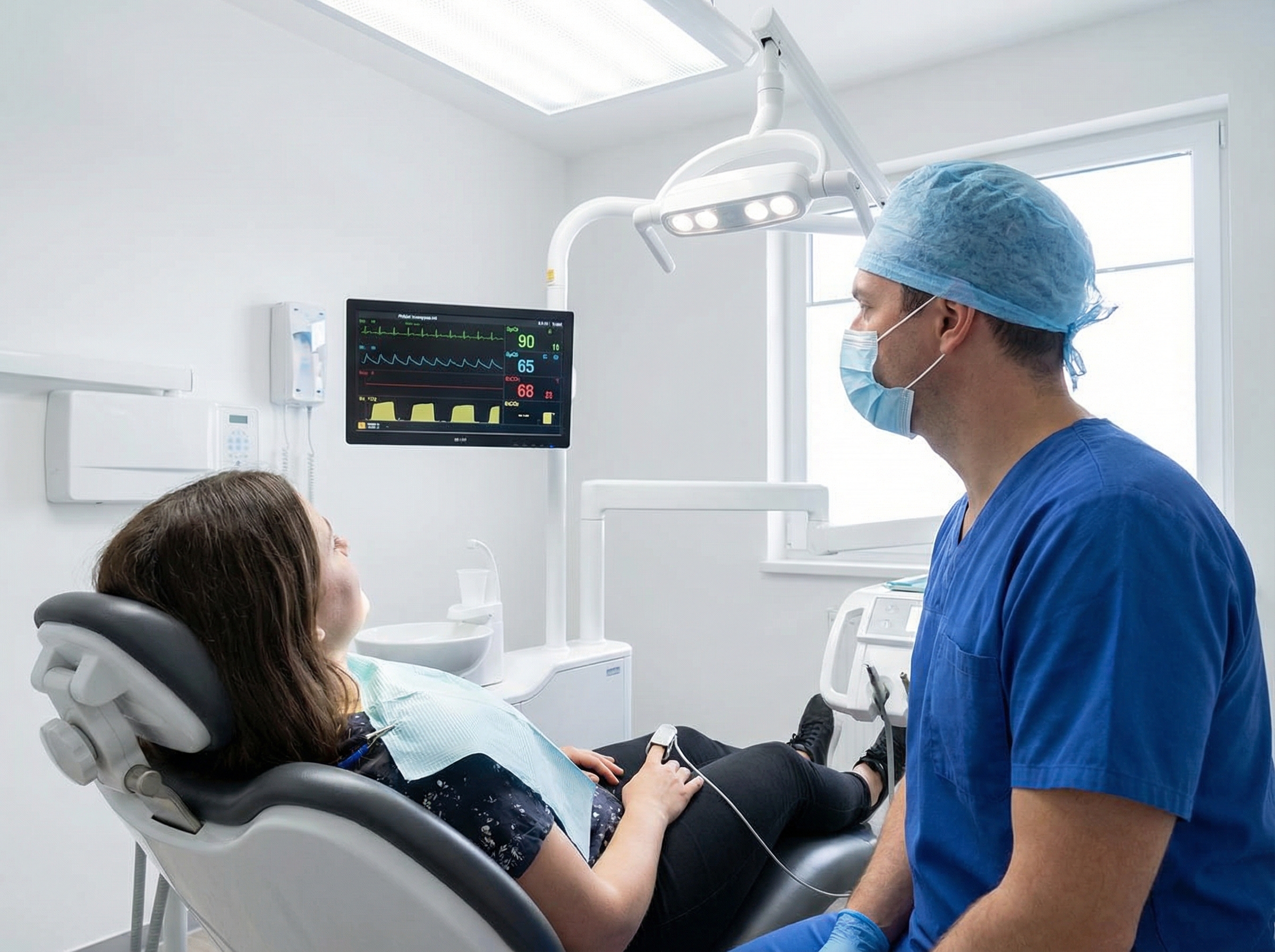
This article walks through the most critical sedation-related emergencies encountered in dental practice, the ACLS skills that directly apply, and why online ACLS certification gives busy dental professionals the training flexibility they need without compromising depth of knowledge. We are practicing emergency physicians who built a certification platform we wished had existed when we were juggling continuing education with full clinical schedules. We understand that dental providers face the same time constraints, and we built our courses accordingly.
Hospital-based providers manage emergencies within a system. Code teams arrive in under two minutes. Crash carts are stocked and checked daily. Respiratory therapists are a phone call away. Dental offices operate in a fundamentally different environment. When a patient decompensates in the chair, the dentist and two or three staff members are the entire response team. Emergency medical services may be five to ten minutes out. The responsibility falls entirely on the people in that room.
Research published by investigators reviewing anesthesia safety in dental settings found that the overall incidence of life-threatening events during dental anesthesia is approximately 2.14 per 10,000 cases, with events directly attributable to anesthesia management occurring at a rate of 0.96 per 10,000 cases. While those numbers may sound low in isolation, dental practitioners in active sedation practices perform hundreds or thousands of cases per year. Across a career, an encounter with a serious adverse event becomes a statistical near-certainty rather than a remote possibility.
Compounding the risk profile is patient complexity. Today's dental sedation patients increasingly arrive with hypertension, coronary artery disease, diabetes, obstructive sleep apnea, and polypharmacy regimens that interact unpredictably with sedative agents. The 2024 research review on best practices in training and preparedness for medical emergencies in dental settings found that standard lecture-based ACLS training alone is insufficient to prepare dental providers for managing real emergencies in their specific clinical environment. Simulation, team drills, and protocol rehearsal are essential complements to certification.
Understanding which emergencies are most likely prepares providers to recognize and act on early warning signs before deterioration becomes irreversible. The following represent the scenarios where ACLS training delivers the most direct clinical benefit.
Benzodiazepines and opioids, the backbone of most dental conscious sedation regimens, produce dose-dependent respiratory depression. In a sedated patient whose protective airway reflexes are blunted, even a modest degree of over-sedation can progress to hypoventilation, hypoxia, and respiratory arrest faster than a pulse oximeter alarm can sound. The dental chair position, combined with a mouth propped open and suction devices in place, creates a uniquely compromised airway geometry compared to a supine ICU patient.
ACLS training directly addresses airway management under these conditions. Providers learn jaw-thrust maneuvers, nasopharyngeal and oropharyngeal airway insertion, and the mechanics of bag-mask ventilation that serves as the critical bridge intervention before EMS arrives or definitive airway management becomes possible. Familiarity with these skills in a low-stakes training environment is the only way to execute them reliably under the pressure of a real event.
For providers administering deeper levels of sedation or general anesthesia, understanding the complete respiratory arrest management pathway is essential. This includes recognizing agonal breathing patterns, understanding oxygen delivery systems, and knowing when to escalate from assisted ventilation to rescue breathing.
Local anesthetics, latex, penicillin-based antibiotics, and NSAID analgesics all carry anaphylaxis potential. In a sedated patient, the classic warning signs of anaphylaxis may be masked or misinterpreted. Erythema dismissed as procedure-related flushing, bronchospasm attributed to anxiety, and hypotension chalked up to the vasodilatory effects of sedation are all documented precursors to delayed epinephrine administration and worse outcomes.
Research published in the PMC review on anaphylaxis management in dental practice confirms that epinephrine must be administered intramuscularly without hesitation at the first clinical recognition of anaphylaxis, with doses of 0.3 to 0.5 mg for adults, repeated as necessary. Antihistamines and corticosteroids are adjuncts, not primary treatments. The ACLS framework for managing anaphylaxis in clinical settings reinforces this priority hierarchy and includes the full escalation pathway through cardiovascular collapse and cardiac arrest if first-line epinephrine fails to reverse the reaction.
Cardiovascular complications span a wide severity spectrum in sedation dentistry. Vasovagal syncope represents the most common event and is generally self-resolving with positioning and observation. But the spectrum extends to hypertensive crises, acute coronary syndromes, serious dysrhythmias, and cardiac arrest, all of which require a tiered response that only ACLS training provides.
Blood pressure fluctuations are the most commonly encountered cardiovascular emergency situations during dental sedation procedures, per published guidelines on sedation and anesthesia administration from the American Society of Anesthesiologists. The ACLS framework provides structured decision-making for distinguishing a compensated hemodynamic perturbation from an evolving catastrophe that requires immediate escalation.
For bradycardia, which can emerge as a vasovagal response, an opioid side effect, or a sign of hypoxic cardiac compromise, the structured approach outlined in the adult bradycardia with a pulse algorithm walks providers through the atropine-first pathway and the escalation to transcutaneous pacing or dopamine infusion when atropine alone proves insufficient. For a dental provider managing this scenario in the chair, having that algorithm internalized is the difference between decisive action and frozen uncertainty.
Cardiac arrest during dental sedation is rare but not unknown. A PMC study on sudden cardiac arrest in dental patients documented cases occurring even in patients awaiting examination, before any procedure had begun. In sedated patients, the respiratory arrest-to-cardiac arrest progression can be devastatingly fast. A patient who moves from oversedation to respiratory failure may experience cardiac arrest within minutes if the airway is not secured and ventilation restored.
ACLS certification prepares dental providers for high-quality CPR delivery, rhythm recognition via AED or monitor, appropriate defibrillation for shockable rhythms, and the pharmacological management of non-shockable rhythms. The comprehensive medication framework, including epinephrine dosing, amiodarone protocols, and the H's and T's differential for reversible causes, is core ACLS content that applies directly in the dental setting. Reviewing the complete ACLS medications cheat sheet during certification training ensures these dosages and indications are fully committed to memory before a real event demands them.
ACLS certification for dental sedation providers is not merely a professional best practice. Across the United States, most state dental boards that regulate moderate sedation, deep sedation, and general anesthesia permits mandate current ACLS certification as a permit condition. The American Society of Anesthesiologists' statement on sedation and anesthesia in dental office-based settings specifies that individuals providing sedation should have successfully completed age-appropriate resuscitative training, with ACLS specifically indicated for adult patient populations.
Beyond the permit requirement, ACLS certification speaks directly to the standard of care analysis in any malpractice action arising from a sedation complication. Providing sedation or general anesthesia without current ACLS certification creates a demonstrable gap between practice and established standard, a gap that becomes particularly consequential when an adverse event results in patient harm. Staying current on ACLS is both a regulatory obligation and a risk management imperative for every dental sedation provider.
The ADA's sedation use guidelines recommend that all personnel involved in the sedation process, not just the administering dentist, maintain appropriate life support training. This means front desk staff should hold current BLS certification, chairside assistants working sedation cases should have BLS at minimum, and the treating dentist should carry valid ACLS. This team-wide certification model is the practice standard endorsed by emergency medicine educators in dental contexts and should be treated as a baseline rather than an aspirational target.
Certification is the foundation, but it is not the whole structure. Research consistently shows that isolated certification training without regular simulation and drills fails to translate into effective emergency performance under pressure. The ACLS-certified dental team that has never practiced its cardiac arrest response together will struggle to function as a cohesive unit when an actual event unfolds in real time.
Effective preparedness requires three elements working together: current certification for all relevant team members, a written emergency protocol posted and rehearsed, and a properly stocked and maintained emergency kit. The protocol should cover role assignments with precision. Who manages the airway? Who operates the AED? Who calls EMS and stays on the line providing updates? Who draws and administers medications? When every person in the room knows their role before the emergency begins, the chaotic silence of a team waiting for direction is replaced by coordinated action that genuinely improves outcomes.
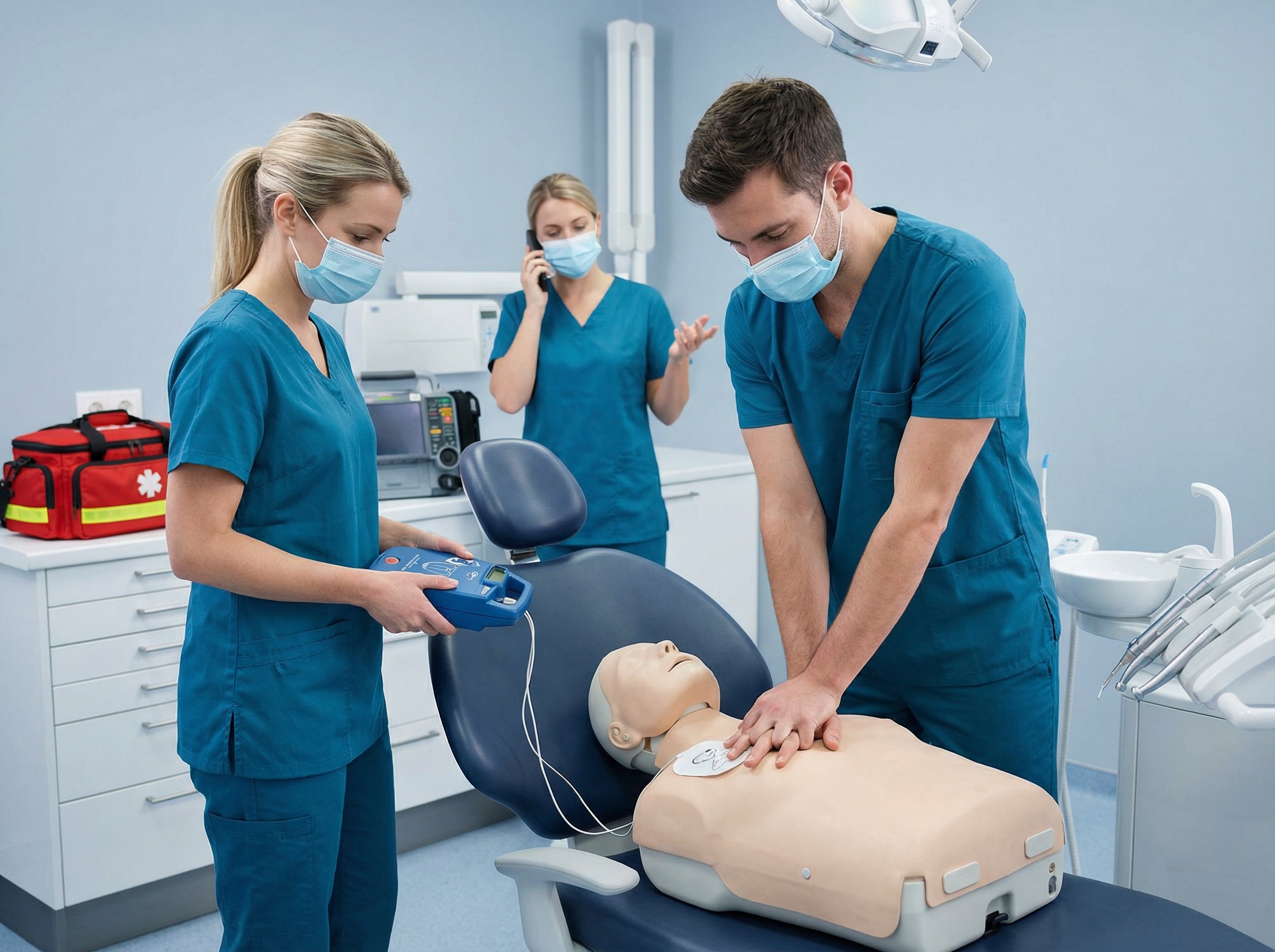
Emergency kit contents should reflect the likely emergencies in the specific practice. A sedation-active office needs epinephrine in multiple doses, atropine, flumazenil for benzodiazepine reversal, naloxone for opioid reversal, nitroglycerin, aspirin, diphenhydramine, and glucose sources alongside BLS adjuncts and a functional AED. The dental practice article on the importance of BLS and ACLS for dental practices covers these foundational elements in detail and is worth sharing with your entire clinical team as a training reference.
Dental providers who perform conscious sedation for procedures are operating in territory that directly overlaps with the core competencies of ACLS. Moderate sedation with benzodiazepines and opioid adjuncts creates conditions where respiratory depression, hemodynamic instability, and cardiovascular events are all plausible. The monitoring standards, the intervention thresholds, and the escalation pathways are ACLS-derived even when they are applied in a dental rather than a hospital context.
Understanding how conscious sedation interacts with cardiovascular physiology helps providers catch early signs of decompensation. The comprehensive review of conscious sedation for cardioversion illustrates the depth of pharmacological and physiological knowledge that ACLS training develops, knowledge that transfers directly to monitoring sedated dental patients for cardiac compromise during procedures.
The pharmacokinetics of midazolam, fentanyl, and ketamine all factor into how quickly a patient can go from appropriately sedated to dangerously oversedated and how rapidly reversal agents need to be administered. ACLS-trained providers understand drug interactions, dosing thresholds, and the physiological consequences of respiratory depression at a level that enables better pre-procedure risk stratification and faster intra-procedure response when warning signs emerge before deterioration accelerates.
The traditional model of in-person ACLS certification has always been a logistical obstacle for dental professionals. A full-day skills station course requires blocking out an entire workday, traveling to a certification center, and navigating scheduling around the rest of the practice calendar. For solo practitioners or small-group practices where the dentist's absence shuts down production, this barrier is significant enough that certifications lapse or renewal gets deferred.
Online ACLS certification through platforms developed by practicing emergency physicians solves this problem directly. The coursework is self-paced, which means a dental provider can complete the didactic content between patient appointments, during a lunch break, or at home in the evening. Immediate digital certification means the provider is credentialed the same day they pass the assessment, a meaningful advantage when a permit renewal deadline or a credentialing application has an imminent due date.
The clinical content in online ACLS courses developed by board-certified emergency medicine physicians is the same ACLS content that applies in the dental operatory. Cardiac arrest algorithms, dysrhythmia management, airway protocols, and ACLS pharmacology are directly relevant to dental sedation emergencies. The knowledge you build completing an online ACLS course at your own pace is the same knowledge you will apply when a patient in your chair stops breathing. The article on why dental practice staff benefit from BLS and ACLS training reinforces this point from the perspective of the full practice team, not just the treating dentist alone.
Affordable ACLS courses are priced at $99 for ACLS certification and $89 for recertification, with BLS available at $59 and $49 for renewal. For a dental practice certifying multiple staff members, bundle pricing and group solutions reduce the per-person cost further. Unlimited retakes ensure that every team member who attempts certification completes it successfully, removing the anxiety of a single high-stakes testing event from an already demanding schedule. These pricing structures exist because financial barriers to certification should never be the reason a dental office faces a preventable emergency without adequate preparation.
Certification provides the cognitive framework. Simulation builds the muscle memory and team coordination that certification alone cannot produce. Published research on medical emergency preparedness in dental settings confirms that providers who have rehearsed emergency scenarios outperform those who have only completed didactic training when confronted with a real or simulated emergency. The team that has practiced the cardiac arrest response knows without being told where the AED is located, who takes over CPR at two minutes, and how to communicate with EMS on arrival.
Quarterly mock drills are the standard recommendation for sedation-active dental offices. Each drill should cover at minimum a cardiac arrest scenario with full CPR and AED deployment, an airway obstruction scenario with bag-mask ventilation, and an anaphylaxis scenario with epinephrine administration and EMS activation. Debriefing after each drill identifies gaps in role clarity, equipment readiness, and clinical skill execution before a real event reveals those same gaps under conditions where the stakes cannot be undone.
The ACLS certification process supports simulation readiness by building the cognitive algorithms that structure emergency response. When a provider has internalized the bradycardia algorithm, the anaphylaxis management sequence, and the cardiac arrest H's and T's framework, their mind is already running the correct decision tree when an emergency begins. Simulation practice converts that cognitive framework into coordinated physical action. The two elements reinforce each other and together produce the caliber of preparedness that genuinely saves patient lives in the dental chair.
Dental sedation in pediatric patients introduces an additional layer of risk and a corresponding obligation for PALS-level knowledge alongside ACLS. Children are not small adults. Their airway anatomy, cardiovascular physiology, and response to sedative agents differ in ways that require specific training to manage safely. The American Academy of Pediatric Dentistry guidelines for sedation monitoring mandate that at least one provider involved in pediatric sedation maintain current PALS certification.
Pediatric patients present with proportionally larger tongues relative to airway size, higher oxygen consumption rates, and more rapid desaturation trajectories than adults. A pediatric patient who begins to desaturate during sedation can reach dangerous hypoxic levels within seconds rather than the minutes that may be available with an adult patient. PALS training prepares dental providers for pediatric weight-based dosing of resuscitation medications, pediatric defibrillation energy requirements, and the modified CPR technique appropriate for infants and children.
Medically complex adult patients, including those with implanted pacemakers, active heart failure, or severe obstructive sleep apnea, also require heightened vigilance during dental sedation. An understanding of how pacemaker function interacts with defibrillation protocols, how heart failure physiology alters the response to fluid loading or vasopressors, and how sleep apnea anatomy creates unpredictable airway collapse under sedation are all areas where ACLS knowledge directly reduces risk for this growing patient population.
ACLS certification carries a two-year expiration for good reason. Resuscitation guidelines are updated as new evidence accumulates, and clinical skills degrade without periodic reinforcement. For dental providers whose exposure to cardiac arrest events may be infrequent even within an active sedation practice, the biennial renewal cycle is the primary mechanism ensuring that algorithms, pharmacology, and skill competency remain at the level patients deserve.
Online recertification makes the renewal cycle far less disruptive to dental practice operations. A self-paced recertification course completed online, with immediate digital certification on successful assessment completion, eliminates the scheduling challenge that historically caused dental providers to let certifications lapse. When state permit renewal cycles align with ACLS expiration dates, current certification needs to be available immediately. Our online platform delivers it the same day you complete the course, with no waiting period and no facility scheduling required.
For dental practices managing certification compliance across a team, group certification solutions simplify the administrative burden significantly. Tracking expiration dates for the dentist, the dental assistants, and any additional sedation-qualified staff becomes manageable when certification can be completed on individual schedules without coordinating group travel to a testing facility. The money-back guarantee on all Affordable ACLS courses removes any remaining barrier from the enrollment decision, ensuring every team member completes the course with full confidence in the training quality they receive.
Every sedation procedure in a dental office is, at some level, a controlled act of physiological manipulation. Providers introduce pharmacological agents that alter consciousness, blunt reflexes, and modify cardiovascular and respiratory dynamics, and they do so in an environment where the safety net of a hospital resuscitation team does not exist. The preparation that replaces that safety net is ACLS training, team drills, emergency protocol development, and an unwavering commitment to staying current on certification.
The dental professionals who fare best in the rare but real moments when sedation turns critical are not necessarily the ones with the most clinical experience. They are the ones who have trained for those moments, who have rehearsed the algorithms, who know which medication to reach for and in what dose, and whose team has practiced the response until coordination becomes automatic. ACLS certification is the foundation of that preparedness, and earning or renewing that certification has never been more accessible or more affordable.
If you are a dental provider who administers sedation, performs general anesthesia, or works alongside colleagues who do, ACLS certification is a professional obligation and a patient safety imperative. Our courses are built by practicing ER physicians who understand what clinical emergencies actually demand, and they are priced to ensure that cost is never a barrier. Enroll today, complete your certification on your own schedule, and walk into your next sedation case with the preparedness every patient in that chair deserves.
.jpg)

